Understanding Cancer
Retinoblastoma
Retinoblastoma, or childhood eye cancer, affects the retina and has a survival rate of 99%
Retinoblastoma overview
Retinoblastoma, also known as eye cancer in children, is a type of cancer that affects the light-sensitive lining at the back of the eye (called the retina) and has a survival rate of 99%.
What is retinoblastoma?
Retinoblastoma is an embryonal tumour and, as such, most cases occur in very young children and babies. It is one of only a very small number of childhood cancers that is caused by a genetic defect inherited from parents.
Retinoblastoma can be either in one eye which is called unilateral, this makes up around two thirds of cases, or in both eyes, which is called bilateral. All children with bilateral tumours have the heritable disease, whereas fewer of unilateral cases have the heritable form. The heritable form of retinoblastoma is now well understood. It occurs as a result of two alterations (called mutations) in the ‘retinoblastoma suppressor gene’ (RB1). The abnormal gene can be passed from a parent to their child, allowing the tumour to develop. Or this alteration can occur spontaneously while the baby is developing in the uterus. Children with the heritable form have an increased risk of developing other types of cancer later in life.
Genetic counselling and support is available for families in which a member has retinoblastoma. Not all children of an affected parent will inherit the faulty gene but all children born into families with a history of retinoblastoma will be screened regularly during their first five years of life for signs so that treatment can be started early if a tumour does develop.
The causes of the non-heritable form of retinoblastoma are not understood.
What are the symptoms of retinoblastoma?
Many of the heritable cases of retinoblastoma will be picked up by screening before any symptoms have been detected.
Where there is no family history, the first sign of retinoblastoma is often a white pupil that does not reflect the light. This is called leucocoria and is sometimes detected in photographs taken using flash photography – the affected eye may look white in the photograph (loss of the red-eye effect). Some children may have a squint or – if the tumour is large – a painful, red eye. In older children, retinoblastoma can be picked up as a result of deteriorating vision.
Incidence
Around 44 children are diagnosed with retinoblastoma every year in the UK. Around two-fifths (40%) of cases are diagnosed in the first year of life and incidence rates drop to a very low rate after five years of age. Around two-thirds (63%) of retinoblastomas are diagnosed in one eye only.
Most of the bilateral cases – which represent just over a third of cases overall – are diagnosed in the first year of life.
Overall, incidence is similar among males and females but there is a male excess of bilateral retinoblastoma (5:4) and a female excess of unilateral retinoblastoma (6:5).
Diagnosis
What would you expect to happen first, when you see your GP?
Diagnosis will be confirmed by an examination under anaesthetic. Unlike most other types of cancer, retinoblastomas can be diagnosed just by their appearance – a biopsy is not usually necessary.
Once retinoblastoma is diagnosed, other tests may be carried out to check the exact position and size of the tumour, and whether it has spread. This is known as staging. These tests may include an ultrasound scan, an MRI scan and a lumbar puncture. A bone marrow sample may be taken to check whether there has been any spread of the cancer to the bone marrow and a blood sample will be taken for genetic testing.
Retinoblastoma can be divided into 5 further subgroups (A to E) depending on the size, position and amount of damage to the eye/s. This helps doctors decide which treatment is best.
Extraocular retinoblastoma is very rare in the UK but means that has spread beyond the eye and into the tissue surrounding it or to other parts of the body.
How is retinoblastoma treated?
Retinoblastoma treatment depends on a number of factors including the staging of the tumour/s. The main aim of treatment is to eradicate the cancer. It may be possible to treat small tumours with laser or freezing treatment called cryotherapy. These procedures are carried out under anaesthetic. Larger tumours are normally shrunk with chemotherapy either given intravenously or in some case by injection into the blood vessel supplying the eye. This is called intraarterial chemotherapy. Other treatments such as direct injection of chemotherapy into the eye and radiotherapy can be used for more complex cases.
Large tumours especially in unilateral cases are often treated with surgery to remove the eye, called enucleation, especially if the sight is already lost and there is no chance of visual recovery. A combination of treatments is often necessary.
What is happening in the body and are there any side effects?
The risk of side effects will depend on the particular treatment being used. Sometimes these can occur years later, called late effects. The child’s doctor will discuss the risks before treatment starts.
The major impact on your child however is vision and the team treating them will endeavour to preserve as much useful vision as possible. Support for visually impaired children will be available including special provisions for schooling
A number of children may develop persistent side effects as a result of treatment, sometimes many years later, these are known as late effects. The most significant of these is the risk of second cancers which is higher in the heritable form of retinoblastoma.
Follow-up
Children will have regular follow-ups to check for any recurrence of the cancer and for any problems which may arise as a result of the treatment they were given.
Following treatment, the child’s eye will be regularly examined by an eye specialist to check that the retina is healthy, the cancer has not come back, and no new tumours have developed.
A small number of children may develop long-term problems because of their cancer treatment.
Surgery and radiotherapy may both cause functional or cosmetic problems. Chemotherapy may cause problems with heart and kidney function, fertility problems and a small increase in risk of developing another cancer.
If the tumour comes back after the initial treatment it is called relapse. Nearly all the children with unilateral tumours survive without any recurrence. However with bilateral disease there is a greater chance it can recur. This recurrence may be in the eye, local tissue surrounding the eye, or in another part of the body.
Children with heritable retinoblastoma will be given genetic counselling when they are old enough to understand.
Children with heritable disease face an increased risk of develop other types of cancer in later life and so will be followed-up into adulthood. They will be encouraged to get any new symptoms checked early and to follow a health lifestyle to help reduce cancer risk.
How effective are the treatments – What are the survival rates?
Nearly all children with retinoblastoma are cured.
Can it come back?
If the tumour comes back after the initial treatment it is called relapse.
Further treatment with chemotherapy, local treatments or enucleation maybe required often a combination of these. It is highly likely a child with recurrent tumour will be cured. The risk of the tumour spreading outside the eye fortunately remains small.
Research
The child may be invited to participate in a clinical trial.
Trials aim to improve understanding of the best way to treat the cancer, usually by comparing the standard treatment with a new or modified version.
Children with Cancer UK is funding a number of research projects focused on retinoblastoma.
Further information
More detailed information about retinoblastoma and its treatment is available from The Childhood Eye Cancer Trust.
Understanding the types of childhood cancer
Each type of childhood cancer has unique characteristics and treatment needs. Here, we provide an overview of the 10 primary types to help you learn more about the various diagnoses that impact young lives.
Topics on this page
- Retinoblastoma
- Retinoblastoma overview
- What is retinoblastoma?
- What are the symptoms of retinoblastoma?
- Incidence
- Diagnosis
- How is retinoblastoma treated?
- What is happening in the body and are there any side effects?
- How effective are the treatments – What are the survival rates?
- Research
- Further information
- Understanding the types of childhood cancer
Related topics
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.

Fundraiser of the Month: Steve and Chris
Fundraiser of the Month: Steve and Chris Our Fundraiser of the Month for June 2026 goes to the incredible Steve…
Read more Fundraiser of the Month: Steve and Chris
Kaiden’s Medulloblastoma Story
Kaiden’s Medulloblastoma Story “I have huge hopes that one day in the future, children like Kaiden can have much kinder…
Read more Kaiden’s Medulloblastoma Story
Too Big Campaign – Press Release
‘2 BIG’: OVERSIZED EVERTON KIT HIGHLIGHTS HARSH REALITY OF CHILDREN RECEIVING ADULT CANCER TREATMENT 11-year-old Kaiden Edwards, who is living…
Read more Too Big Campaign – Press Release
Fundraiser of the Month: Izzy
Fundraiser of the Month: Izzy Our Fundraiser of the Month for April 2026 goes to the amazing Izzy, who set…
Read more Fundraiser of the Month: Izzy
Teenage and Young Adult Cancer Awareness Month 2026
Childhood cancer survivor shares his story for Teenage and Young Adult Cancer Awareness Month after completing a marathon and inspiring others to follow.
Read more Teenage and Young Adult Cancer Awareness Month 2026
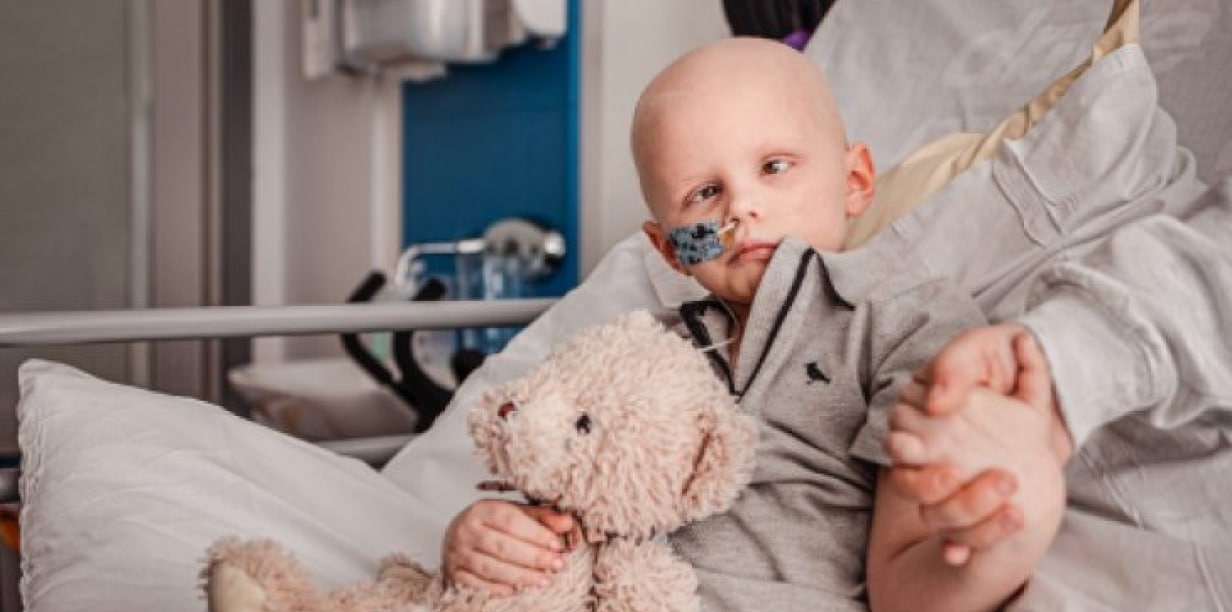
Alfie’s Glioblastoma Story
Alfie’s Glioblastoma Story Alfie was only 3 months old when his dad noticed something wasn’t right. Read his full story…
Read more Alfie’s Glioblastoma Story
Teddy’s Leukaemia Story
Teddy’s Leukaemia Story Teddy was only 3 when he was diagnosed with Leukaemia. His father, Sam is sharing Teddy’s story…
Read more Teddy’s Leukaemia Story
2026 Research Grant Call launched
Children with Cancer UK launches the 2026 Research Grant Call to accelerate breakthroughs in childhood cancer
Read more 2026 Research Grant Call launched
Emil’s Brain Tumour Story
Emil’s Brain Tumour Story Hear Emil tell his story of his brain tumour diagnosis when he was 9 and how…
Read more Emil’s Brain Tumour Story
Ren’s Neuroblastoma Story
Ren’s Neuroblastoma Story Ren was diagnosed with Neuroblastoma at just eight months old. His mum Harriot is sharing his story….
Read more Ren’s Neuroblastoma Story