Childhood Cancer Info
Commonly Used Terms
Below are some of the terms commonly used when talking about the treatment of childhood cancer. Click on the term to reveal the explanation.
A benign tumour is not cancerous. It may, however, still cause problems depending on its location.
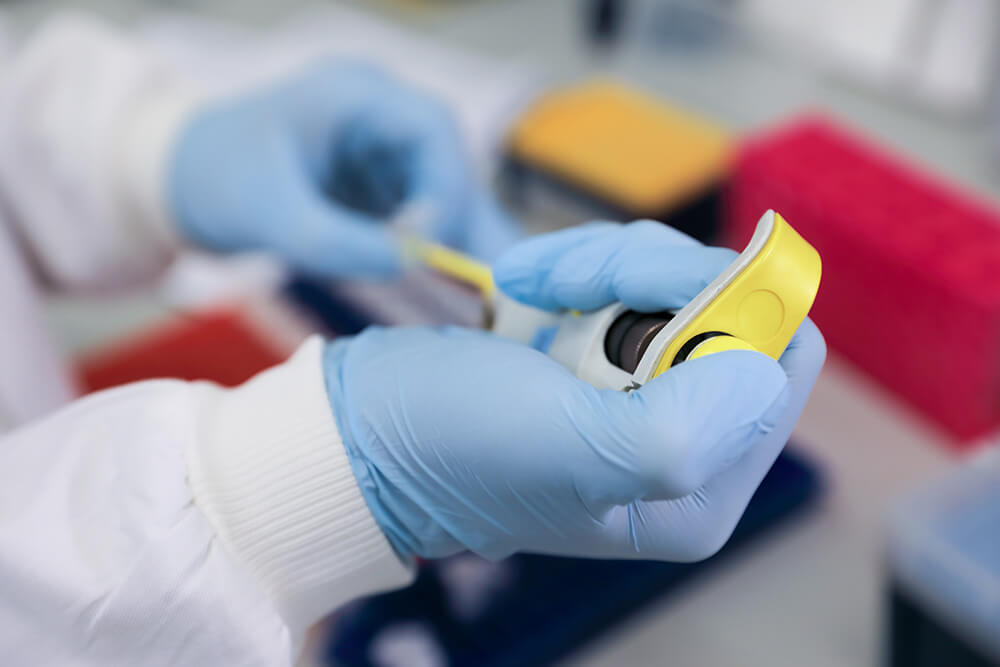
If doctors suspect that a tumour is cancerous, a surgeon may remove part of it to examine under a microscope. This may either been done by a needle, which is put into the tumour through the skin to remove a sample of cells, or by open biopsy, where a small piece of the tumour is taken during a small operation. The cells will be sent to a laboratory for examination; the results may take several days.
Bone marrow transplantation is the term previously used to describe stem cell transplantation – see below. The new terminology reflects the less invasive method now used to collect stem cells from the donor’s circulating blood rather than their bone marrow.
A central line is a tube which is used to give chemotherapy. It goes into the chest and directly into one of the major blood vessels. It usually stays in place for the duration of treatment. The end of the central line protrudes from the chest and is sealed off with a cap. Having a central line avoids the needs for repeated injections as all intravenous medication can be given through the line. The line can also be used to collect blood samples which are frequently required during treatment.
Chemotherapy is the term used to describe the drugs which a child is given to kill the cancer cells. These drugs may be taken orally (by mouth), intravenously (injected directly into a vein), intramuscularly (injected directly into the muscle) or intrathecally (directly into the spinal fluid via a lumbar puncture).
A CT scan shows up areas of the inside of the body. The CT scanner takes a series of X-rays from different angles. A computer uses the x-rays to build up a 3D picture of the inside of the body. CT scans are painless but the child may be given a sedative or general anaesthetic to make sure that they lie still.
DLI is a treatment used in leukaemia patients who have relapsed following a stem cell (also known as bone marrow) transplant. The procedure uses lymphocytes (white blood cells) from the same donor to boost the life-saving effects of the original transplant.
Hickman line is another term for ‘central line’ – see above.
Histology refers to the microscopic anatomy of cells and tissues. When cells or tissues are taken by biopsy, they are examined under a microscope to aid diagnosis.
Lumbar puncture is a procedure whereby a needle is inserted into the lower part of the spine to take a sample of fluid. The fluid is known as cerebrospinal fluid (CSF) and it can be tested to look for evidence of cancer cells, infection, and raised pressure in the central nervous system. It can also be used to inject chemotherapy into the cerebrospinal fluid, called intra-thecal treatment. This can be done under general anaesthetic in very young children, as they need to lie very still. Teenagers may be able to tolerate the procedure using local anaesthetic to numb the skin.
A malignant tumour is cancerous. If a tumour is malignant it grows uncontrollably and can travel to other parts of the body.
Metastases (also known as secondary tumours) are tumours that have spread from a first (primary) tumour in another part of the body.
Definition
Minimal residual disease (MRD) is the term used to describe the presence of residual cancer cells, when there are so few present that they cannot be detected by routine means. When a child is first diagnosed with leukaemia they may have as many as one million million leukaemic cells in their blood and bone marrow. This level of disease can be easily detected by examining a blood or bone marrow sample under a microscope. The aim of the first stage of treatment is to reduce the burden of leukaemic cells to a level which allows production of normal blood cells to resume. A child is said to be in remission when they reach this point. However a child in remission may still have as many as one thousand million leukaemic cells in their body. This is known as minimal residual disease (MRD). This level of disease cannot be readily detected under the microscope. Every child is given further treatment in order to completely eradicate the disease from their body.
A breakthrough in treatment
It is important to know how much leukaemia is still present in a child’s blood and bone marrow at remission because this helps to predict how likely it is that the child will relapse. Until recently doctors did not have an accurate method for measuring MRD. But many years of research have culminated in the development of a breakthrough molecular technique for measuring MRD. Use of this new MRD test formed the basis of the successful national clinical trial for childhood ALL – UK ALL 2003. Doctors used the test to assess relapse risk in more than 2,500 children undergoing treatment for ALL. This enabled them to tailor each child’s treatment to their individual needs. The aim was not only to improve the chance of cure in high-risk children but to reduce toxicity in low-risk children by not giving them more treatment than they needed.
MRD testing adopted by NHS
The trial was so successful that the NHS has now adopted MRD testing as part of the standard treatment regime for children with ALL. It is thought that this innovation may drive the survival rate for childhood ALL above 90%. Children with Cancer UK invested more than £3 million in this ground-breaking work. The ongoing costs of MRD testing will now be borne by the NHS.
An MRI scan is similar to a CT scan (see above) but uses magnetism instead of X-rays to build up the pictures. The scan is painless but it can be frightening as the machine is very noisy and the child has to lie in a narrow tunnel. The child may be given a sedative or a general anaesthetic to make sure that they lie still. They will also be given earplugs or headphones to wear.
A portacath is a small chamber or reservoir that sits under the patient’s skin at the end of their central line. Chemotherapy drugs are given by inserting a needle into the chamber. The portacath stays in place for as long as treatment is needed. The main advantage of a portacath is that it is not visible on the outside of the body. There is no tube coming out of the chest, as there is with a central line. But some people prefer a central line because they don’t like having a needle put in each time they need treatment. It is possible to have the area over the portacath numbed with a local anaesthetic cream before the needle is put in.
A PET scan uses low-dose radioactive glucose to measure the activity of cells in different parts of the body. A very small amount of a mildly radioactive substance is injected into a vein, usually in the arm. A scan is taken a couple of hours later. Areas of cancer show up on the scan because they are usually more active than surrounding tissue.
Proton beam therapy is an advanced form of radiotherapy that uses a precision high-energy beam of particles (protons) to destroy cancer cells. Because it is so much more precise than conventional radiotherapy, proton beam therapy delivers a high-dose of radiation to the tumour whilst sparing surrounding healthy tissue. This makes it particularly beneficial for children because it reduces the potential for both short-term side effects and long-term impairments. However, the treatment is not a ‘magic bullet’ and further scientific and clinical research is required in order to properly assess its safety and effectiveness in treating different types of cancer. There are currently no proton beam therapy facilities available in the UK but in cases where doctors believe that a patient will benefit, the NHS will fund treatment abroad, usually in the US. In the recent high profile case of Ashya King, his doctors did not believe that proton beam therapy would be beneficial. In 2015 the government pledged to build two NHS proton beam centres, one in London and one in Manchester. These are due to be operational by 2018. In the meantime, a private health company is due to open a centre in Cardiff by December 2016 and two further centres, in London and Northumberland, the following year. These private centres will be available to NHS patients as an alternative to going abroad for treatment.
Radiotherapy treats cancer by using high-energy rays to destroy the cancer cells in one area of the body, while doing as little harm as possible to healthy cells. The treatment is usually given as a series of short daily sessions over a few weeks. Radiotherapy is also used in children with leukaemia who require a stem cell (bone marrow) transplant. Radiotherapy is used to destroy their existing bone marrow prior to transplantation.
A child is said to have relapsed if their cancer returns once they have achieved remission. Treatment options for children who relapse will be determined by a number of factors.
A child is said to have achieved remission when there is no evidence of the disease using standard tests. There may still be minimal residual disease present at remission (see minimal residual disease, above), hence the need for further blocks of treatment.
A stem cell – or bone marrow – transplant allows children to have much higher doses of chemotherapy than they could otherwise tolerate. This improves the chances of curing their cancer but has more side effects. Very high doses of chemotherapy destroy the blood stem cells in bone marrow, so after high-dose chemotherapy a child will be given stem cells as a drip. These make their way to the bone marrow and start producing blood cells again. Stem cell transplants can also bring about an important curative effect in leukaemia patients, known as graft versus leukaemia.
Surgery plays a very important part in the treatment of cancer. Depending on the size and position of the tumour in the body, an operation to remove it may be the first part of treatment. Sometimes, surgery may be dangerous or cause too much damage because of the size and position of the tumour. In these situations, chemotherapy or radiotherapy may first be used to shrink the tumour.
A tumour marker is a substance found in the blood, urine or body tissues that can be elevated in cancer. Tumour markers can be produced directly by the tumour or by non-tumour cells as a response to the presence of a tumour. Tumour markers can be used to detect tumours via screening programmes for common cancers; they can be used to monitor cancer survivors after treatment by detecting recurrence; and they can be used for diagnosis of specific tumour types, particularly in cases where biopsy is not feasible, such as brain tumours.
An ultrasound scan uses sound waves to build up a picture of the inside of the body. A gel will be spread onto the part of the body being scanned. A small hand-held device, like a microphone, which produces sound waves, is passed over the area. The sound waves are then converted into a picture by a computer. Ultrasound scans are used particularly to look at the abdomen and heart.
RESEARCH PROJECTS
Cancer is the leading cause of death in children aged 1-14 years in the UK and survivors can face a lifetime of serious health issues as a result of the intensive treatments used to treat their cancer. Childhood cancers are different to the cancers that occur in adults – dedicated research is needed. Would you like to help?
Stay in touch
Stay up to date with all our research news, exclusive stories, fundraising events and opportunities to support us.
"*" indicates required fields
By signing up to this newsletter i agree to the privacy policy and to receive general and financial appeal emails from children with cancer uk.
Related topics
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.

Teenage and Young Adult Cancer Awareness Month 2026
Throughout April, we’ll be sharing stories from young people about the impact of cancer on fertility, body image, mental health and education, to amplify their voices and raise awareness of their experiences.
Read more Teenage and Young Adult Cancer Awareness Month 2026
Mother’s Day
Mother’s Day We recently told you Leah’s story. After being told that her body would never be able to carry…
Read more Mother’s Day
National Cancer Plan
National Cancer Plan: A welcome vision born from tragedy, but families need support today 4 February 2026 The National Cancer…
Read more National Cancer Plan
World Cancer Day 2026
World Cancer Day 2026 What is World Cancer Day? World Cancer Day takes place on February 4th every year. The…
Read more World Cancer Day 2026
More Child Research is Needed
2 Children received a terminal cancer diagnosis today. In 2026, this should’t happen. Only around 2% of cancer research funding…
Read more More Child Research is Needed
Childhood Cancer Research
Real research. Real breakthroughs. Real children who’ll benefit. Every contribution brings us one step closer to better young person’s treatments,…
Read more Childhood Cancer Research
Thank you for your support
Surviving childhood cancer is just the beginning Every contribution brings us one step closer to better young person’s treatments, improved…
Read more Thank you for your support
Childhood Cancer Treatment
Our children deserve cancer treatments designed for them. Every contribution brings us one step closer to more effective young person’s…
Read more Childhood Cancer Treatment
Childhood Cancer Report
FREE Childhood Cancer Report Only around 2% of cancer research funding in the UK* is spent on research that is…
Read more Childhood Cancer ReportOur Annual Reports
OUR ANNUAL REPORTS Each year we publish an impact report highlighting key areas of our work within childhood cancer research….
Read more Our Annual Reports