Understanding Cancer
Germ Cell Cancer
Germ cell cancer is a rare group of cancers that develop from reproductive cells. Germ cell ovarian cancer typically forms in the ovaries and is one of the main types of gonadal germ cell tumours. Families affected can access dedicated support services and learn how to donate to fund vital research and care, helping improve outcomes for children and young people facing these diagnoses.
About childhood germ cell tumours
Germ cell tumours (GCT) are a diverse group of tumours that usually develop within the ovaries or testes. These are called gonadal germ cell tumours.
However, germ cell tumours can also occur in other parts of the body. As a baby develops in the womb, the germ cells usually move to the ovaries or testes. Sometimes they fail to migrate to their proper location and settle in other parts of the body, where they can develop into tumours. These are called extragonadal germ cell tumours. The most common places for these tumours to occur are at the bottom of the spine called a sacrococcygeal, the brain, chest and abdomen.
There are several distinct sub-types of germ cell tumour, depending on the characteristics of the cells involved. These include yolk-sac tumours, germinomas, embryonal carcinomas and teratomas. They may be benign or malignant.
What are the symptoms of germ cell tumours?
The symptoms depend on where the germ cell tumour develops, but usually a lump appears that can either be felt or leads to other problems such as chest or abdominal pain. The tumour may press on adjacent structures, such as the bladder causing excessive urination.
Incidence
Germ cell tumours and gondal tumours are rare, accounting for around 4% of childhood cancer registrations. This represents about 55 children a year in the UK.
The pattern by age and sex varies greatly according to the type of tumour. In boys, incidence peaks very early at around two years of age and then declines before rising again in adolescence. In girls, incidence is low until age 6 or 7 years and then rises with age up to 15 years.
Diagnosis
What would you expect to happen first, when you see your GP?
A variety of tests and investigations may be needed to diagnose a germ cell tumour.
A biopsy is likely to be taken; this will help to determine the precise type of tumour and whether it is malignant or benign. A CT or MRI scan will enable doctors to determine the exact position of the tumour. Chest x-rays may be taken to check whether the cancer has spread to the lungs.
Germ cell tumours often produce proteins that can be measured in the blood. These proteins are alpha fetoprotein (AFP) and human chorionic gonadotrophin (HCG) and are known as tumour markers. The levels of these proteins will be checked when the tumour is diagnosed and will be monitored during and after treatment. Sometimes the presence of these markers is enough to diagnose a GCT and a biopsy is not needed.
Staging
The ‘stage’ of a cancer is a term used to describe its size and whether it has spread beyond its original site. Knowing the particular type and stage of the cancer helps doctors to decide on the most appropriate treatment. Generally, cancer is divided into four stages:
- Stage 1: the cancer is small and has not spread and has been completely removed.
- Stages 2 and 3: the cancer is larger and may not have been completely removed or may have spread to nearby organs.
- Stage 4: the cancer has spread to other parts of the body. Cancer that has spread to distant parts of the body and formed new tumours is known as secondary or metastatic cancer
Treatment
Treatment depends on the staging, size and position of the tumour.
The principal treatment for germ cell tumours is surgery, except where the tumour is in the brain or spinal cord. If the tumour is benign or if it is malignant but localised and has not spread, then surgery alone may be sufficient. Surgery may involve the removal of the testis or ovary if this is where the tumour first developed.
In cases where the tumour has spread, or if it can’t be easily or completely removed, chemotherapy will be given before and after surgery. Germ cell tumours are very sensitive to chemotherapy and a combination of drugs is usually used over a few months.
Tumours in the brain are sensitive to chemotherapy but may also be treated with radiotherapy.
What is happening in the body and are there any side effects?
Treatment for germ cell cancer often causes side effects and these will be discussed before treatment starts.
The possible side effects of chemotherapy depend upon the drugs used but may include
- nausea and vomiting,
- hair loss,
- reduced resistance to infection,
- bruising and
- bleeding,
- tiredness and
- diarrhoea.
These problems are all temporary and can be minimised with good supportive care.
A number of children may develop persistent side effects as a result of treatment, sometimes many years later, these are known as late effects. These can include
- a small increase in the risk of developing a second cancer later in life
- a reduction in normal bone growth
- reduced fertility
- a change in heart function
Follow-up
The outlook for children with germ cell tumours is good.Children will have regular follow-ups to check for any recurrence of the cancer and for any problems which may arise as a result of the treatment they were given. A small number of children may develop long-term problems because of their germ cell cancer treatment. Surgery and radiotherapy may both cause functional or cosmetic problems depending on the area of the body in which the tumour occurred. Removal of a single ovary or testis should not affect a child’s future ability to have children. Chemotherapy may cause problems with heart and kidney function, fertility problems and a small increase in risk of developing another cancer. Occasionally, the cancer can recur. This is called a relapse. Relapse occurs most likely as a result of a few of the original cancer cells surviving the treatment. Sometimes, this is because cancer cells spread to other parts of the body and were too small to be detected during the follow-up immediately after treatment.The treatment and prognosis for relapsed disease will depend on a number of factors including the site of relapse.
Survival Rate
How effective are the treatments – What are the survival rates?
The overall survival rate for children diagnosed with germ cell cancer is good. Further support for the long term effects of the disease and treatment may be required. Children will have regular follow-ups to check for any recurrence of the cancer and for any problems which may arise as a result of the treatment they were given.

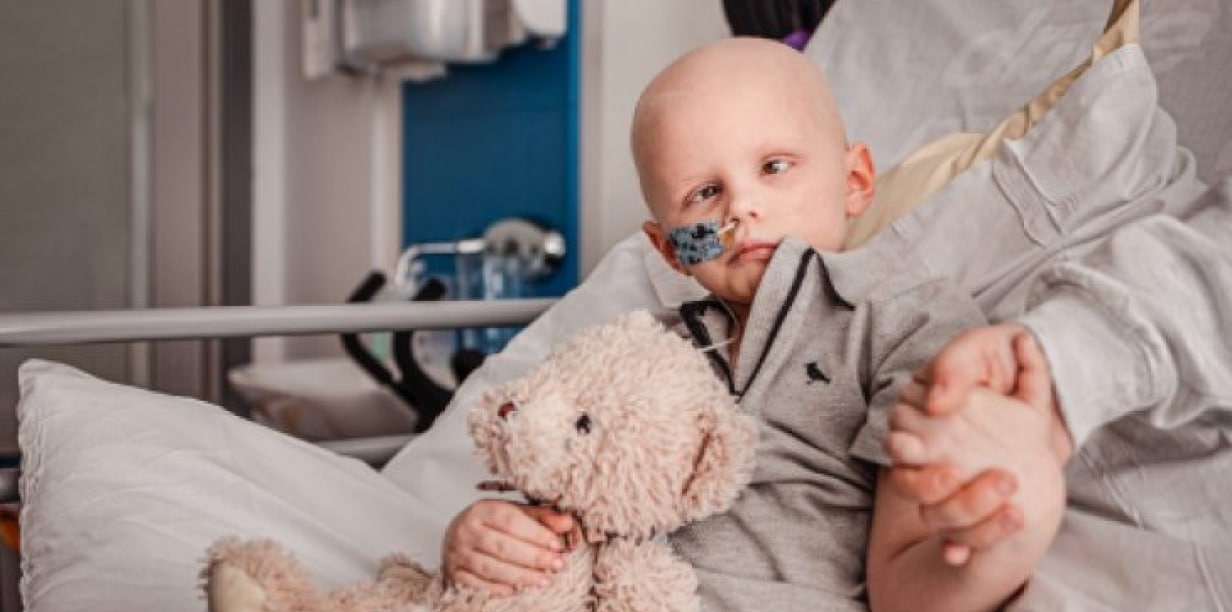
Read Tattianah’s story
Tattianah was diagnosed with an immature teratoma, a type of germ cell tumour, in 2019, when she was just three months old.
Can it come back?
Occasionally, the cancer can recur. This is called a relapse. Relapse occurs most likely as a result of a few of the original cancer cells surviving the treatment. Sometimes, this is because cancer cells spread to other parts of the body and were too small to be detected during the follow-up immediately after treatment.
The treatment and prognosis for relapsed disease will depend on a number of factors including the site of relapse.
Understanding the types of childhood cancer
Each type of childhood cancer has unique characteristics and treatment needs. Here, we provide an overview of the 10 primary types to help you learn more about the various diagnoses that impact young lives.
Topics on this page
- Germ Cell Cancer
- About childhood germ cell tumours
- What are the symptoms of germ cell tumours?
- Incidence
- Diagnosis
- Staging
- Treatment
- What is happening in the body and are there any side effects?
- Follow-up
- Survival Rate
- Read Tattianah’s story
- Can it come back?
- Understanding the types of childhood cancer
Related topics
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.

Fundraiser of the Month: Izzy
Fundraiser of the Month: Izzy Our Fundraiser of the Month for April 2026 goes to the amazing Izzy, who set…
Read more Fundraiser of the Month: Izzy
Teenage and Young Adult Cancer Awareness Month 2026
Childhood cancer survivor shares his story for Teenage and Young Adult Cancer Awareness Month after completing a marathon and inspiring others to follow.
Read more Teenage and Young Adult Cancer Awareness Month 2026
Alfie’s Glioblastoma Story
Alfie’s Glioblastoma Story Alfie was only 3 months old when his dad noticed something wasn’t right. Read his full story…
Read more Alfie’s Glioblastoma Story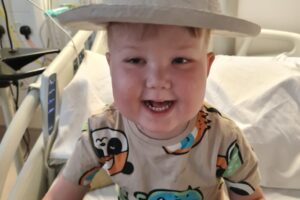
Teddy’s Leukaemia Story
Teddy’s Leukaemia Story Teddy was only 3 when he was diagnosed with Leukaemia. His father, Sam is sharing Teddy’s story…
Read more Teddy’s Leukaemia Story
2026 Research Grant Call launched
Children with Cancer UK launches the 2026 Research Grant Call to accelerate breakthroughs in childhood cancer
Read more 2026 Research Grant Call launched
Emil’s Brain Tumour Story
Emil’s Brain Tumour Story Hear Emil tell his story of his brain tumour diagnosis when he was 9 and how…
Read more Emil’s Brain Tumour Story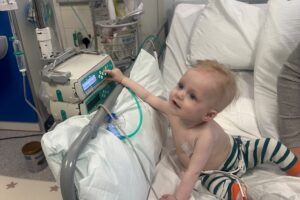
Ren’s Neuroblastoma Story
Ren’s Neuroblastoma Story Ren was diagnosed with Neuroblastoma at just eight months old. His mum Harriot is sharing his story….
Read more Ren’s Neuroblastoma Story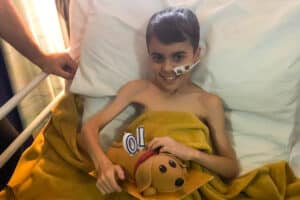
Brain Tumour Awareness Month
Children with Cancer UK is raising awareness & funding new research to deliver more targeted treatment for children with brain tumours
Read more Brain Tumour Awareness Month
Fundraiser of the Month: Darragh
Fundraiser of the Month: Darragh Our Fundraiser of the Month for March 2026 goes to Darragh, who took on the…
Read more Fundraiser of the Month: Darragh
Patient Story – Daithi
Daithi’s Story: Living with Neuroblastoma Daithi was diagnosed with neuroblastoma, a rare childhood cancer. His parents, Gemma and Connor, tell his…
Read more Patient Story – Daithi