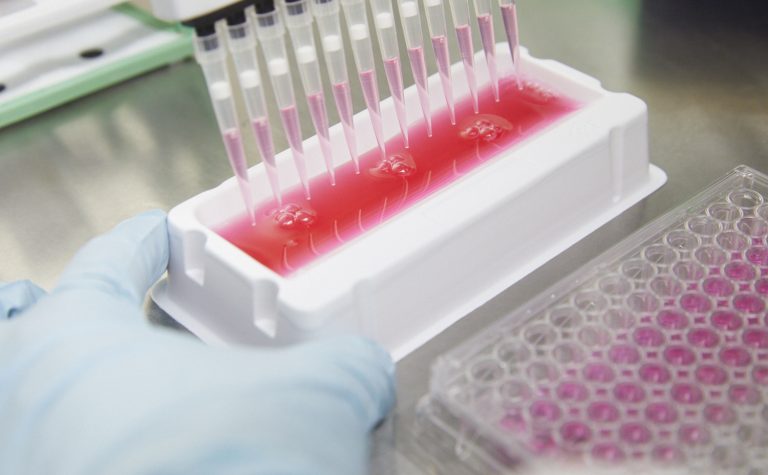
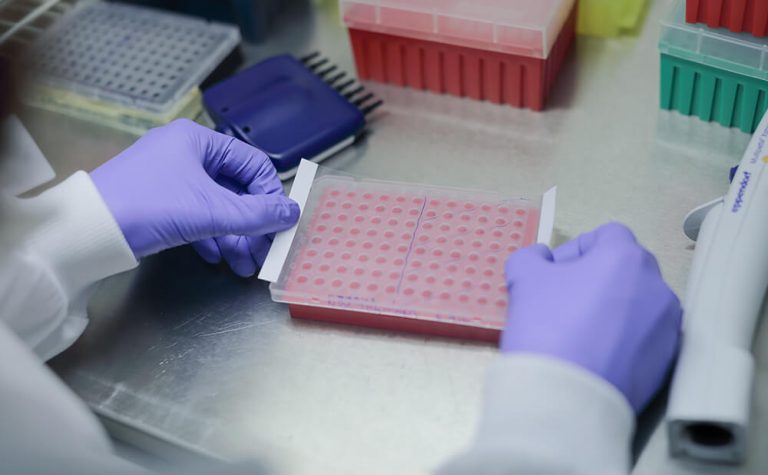
Although many children with Wilms’ tumour are successfully treated with a combination of surgery and chemotherapy, some are still dying from this disease. There is an urgent need to know more about why it develops, so the team is investigating the very basic biology of these tumours to help predict disease outcomes and enable doctors to tailor treatments to individual children.
We’re funding this project to learn more about why Wilms’ tumour develops, so we can predict its development and address an urgent need for new treatments that can be tailored to each child’s needs. Read Niamh’s kidney cancer story to learn how cancer research helped her overcome Wilms tumour.
Thank you
This research project on Wilms’ tumour has been successfully completed. Your donations allow us to fund ground-breaking research that can improve treatments given to children with cancer. Thank you. Your help allows us to continue to find ways to drive up the chances of survival for children with cancer and reduce the toxic side effects that can affect the rest of their lives.