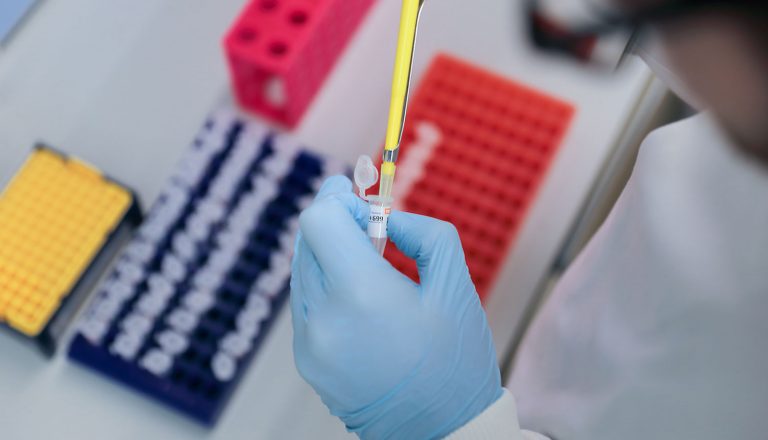
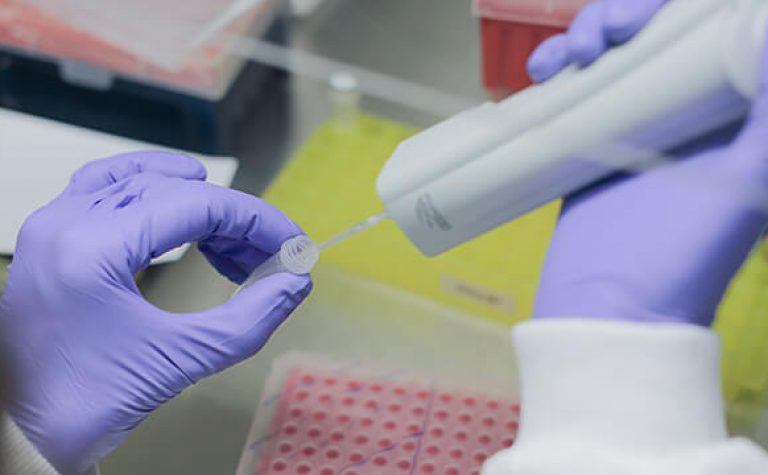
Some children are affected by a kind of neuroblastoma that we can’t cure, as it spreads around the body and none of the treatments work. Professor Louis is doing vital research into how and why it develops and resists treatment, so we can start to look for new ways of to treat and eventually cure children with this disease.
Before we can work towards treatments for incurable childhood cancers like high-risk neuroblastoma, we need to understand how they spread, and why the current drugs don’t work. Professor Louis’s project will help us learn more.
Thank you
This research project on high-risk neuroblastoma has been successfully completed. Your donations allow us to fund ground-breaking research that can improve treatments given to children with cancer. Thank you. Your help allows us to continue to find ways to drive up the chances of survival for children with cancer and reduce the toxic side effects that can affect the rest of their lives.