Childhood Cancer Info
Minimal residual disease in children
MRD or Minimal Residual Disease refers to a level of leukaemia in which there are less than one thousand million cancer cells in the body and therefore cannot be detected by a microscope. A patient in remission (no symptoms) after treatment may still have MRD causing the cancer to relapse
What is Minimal Residual Disease?
When a child is first diagnosed with leukaemia they may have as many as one million million leukaemic cells in their blood and bone marrow. This level of disease can be easily detected by examining a blood or bone marrow sample under a microscope. The aim of the first stage of treatment is to reduce the burden of leukaemic cells to a level which allows production of normal blood cells to resume. A child is said to be in remission when they reach this point. However a child in remission may still have as many as one thousand million leukaemic cells in their body. This is known as minimal residual disease (MRD). This level of disease cannot be readily detected under the microscope. Every child is given further treatment in order to completely eradicate the disease from their body.
A breakthrough in treatment
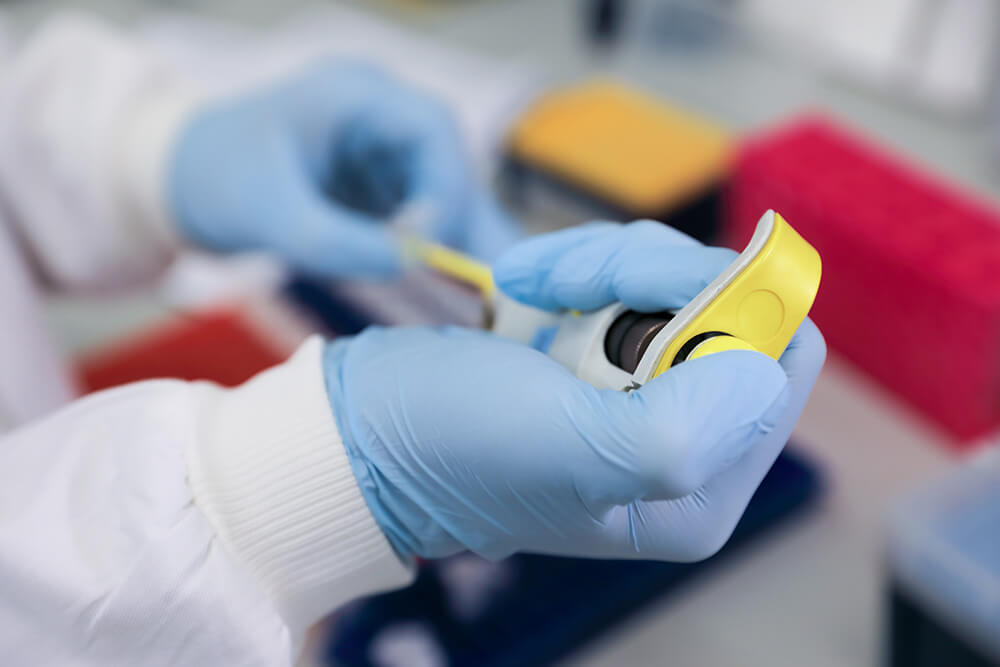
It is important to know how much leukaemia is still present in a child’s blood and bone marrow at remission because this helps to predict how likely it is that the child will relapse. Until recently doctors did not have an accurate method for measuring MRD. But many years of research have culminated in the development of a breakthrough molecular technique for measuring MRD.

Use of this new MRD test formed the basis of the most recent national clinical trial for childhood ALL – UK ALL 2003. Doctors used the test to assess relapse risk in more than 2,500 children undergoing treatment for ALL. This enabled them to tailor each child’s treatment to their individual needs. The aim was not only to improve the chance of cure in high-risk children but to reduce toxicity in low-risk children by not giving them more treatment than they needed. As Dr Nick Goulden, Consultant Paediatric Haematologist at Great Ormond Street Hospital, explains: “When you’re treating children, the most important thing is to do as little harm as possible. Chemotherapy does have side effects – both in the short-term and in the long-term. Anything that allows us to get the same cure rates but reduce toxicity has to be a good thing.”
MRD testing adopted by NHS
The trial was so successful that the NHS has now adopted MRD testing as part of the standard treatment regime for children with ALL. It is thought that this innovation may drive the survival rate for childhood ALL above 90%. Children with Cancer UK invested more than £3 million in this ground-breaking work. The ongoing costs of MRD testing will now be borne by the NHS.
Topics on this page
- Minimal residual disease in children
- What is Minimal Residual Disease?
- A breakthrough in treatment
- MRD testing adopted by NHS
Related topics
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.

Teenage and Young Adult Cancer Awareness Month 2026
Throughout April, we’ll be sharing stories from young people about the impact of cancer on fertility, body image, mental health and education, to amplify their voices and raise awareness of their experiences.
Read more Teenage and Young Adult Cancer Awareness Month 2026
Mother’s Day
Mother’s Day We recently told you Leah’s story. After being told that her body would never be able to carry…
Read more Mother’s Day
National Cancer Plan
National Cancer Plan: A welcome vision born from tragedy, but families need support today 4 February 2026 The National Cancer…
Read more National Cancer Plan
World Cancer Day 2026
World Cancer Day 2026 What is World Cancer Day? World Cancer Day takes place on February 4th every year. The…
Read more World Cancer Day 2026
More Child Research is Needed
2 Children received a terminal cancer diagnosis today. In 2026, this should’t happen. Only around 2% of cancer research funding…
Read more More Child Research is Needed
Childhood Cancer Research
Real research. Real breakthroughs. Real children who’ll benefit. Every contribution brings us one step closer to better young person’s treatments,…
Read more Childhood Cancer Research
Thank you for your support
Surviving childhood cancer is just the beginning Every contribution brings us one step closer to better young person’s treatments, improved…
Read more Thank you for your support
Childhood Cancer Treatment
Our children deserve cancer treatments designed for them. Every contribution brings us one step closer to more effective young person’s…
Read more Childhood Cancer Treatment
Childhood Cancer Report
FREE Childhood Cancer Report Only around 2% of cancer research funding in the UK* is spent on research that is…
Read more Childhood Cancer ReportOur Annual Reports
OUR ANNUAL REPORTS Each year we publish an impact report highlighting key areas of our work within childhood cancer research….
Read more Our Annual Reports