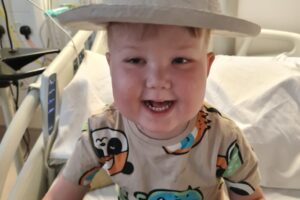
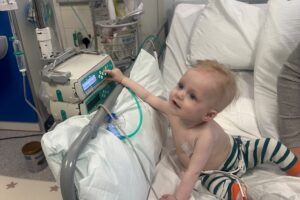
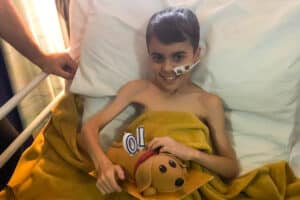
Archer’s Neuroblastoma Story
Archer was diagnosed with high-risk neuroblastoma on 30 December 2021 when he was just two years old. His mum Jade tells their story so far: Support children like Archer so that they have a future they deserve.
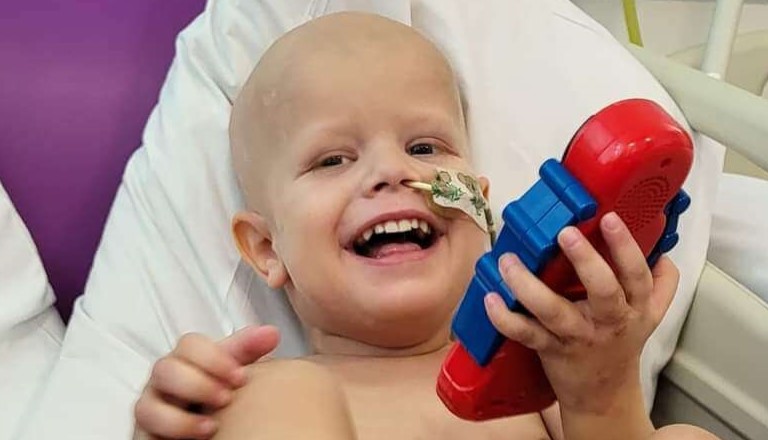
He developed a phobia of water
In the run up to diagnosis, a lot of Archer’s symptoms could be put down to a toddler who had experienced lockdown. He was very clingy to me, his mum, he would take one bite of food and say he was full before moving onto the next thing. He was getting increasingly shyer and more subdued, started to get more tired, and weirdly he developed a phobia of water, which was later attributed to how the tumour was affecting his adrenaline.

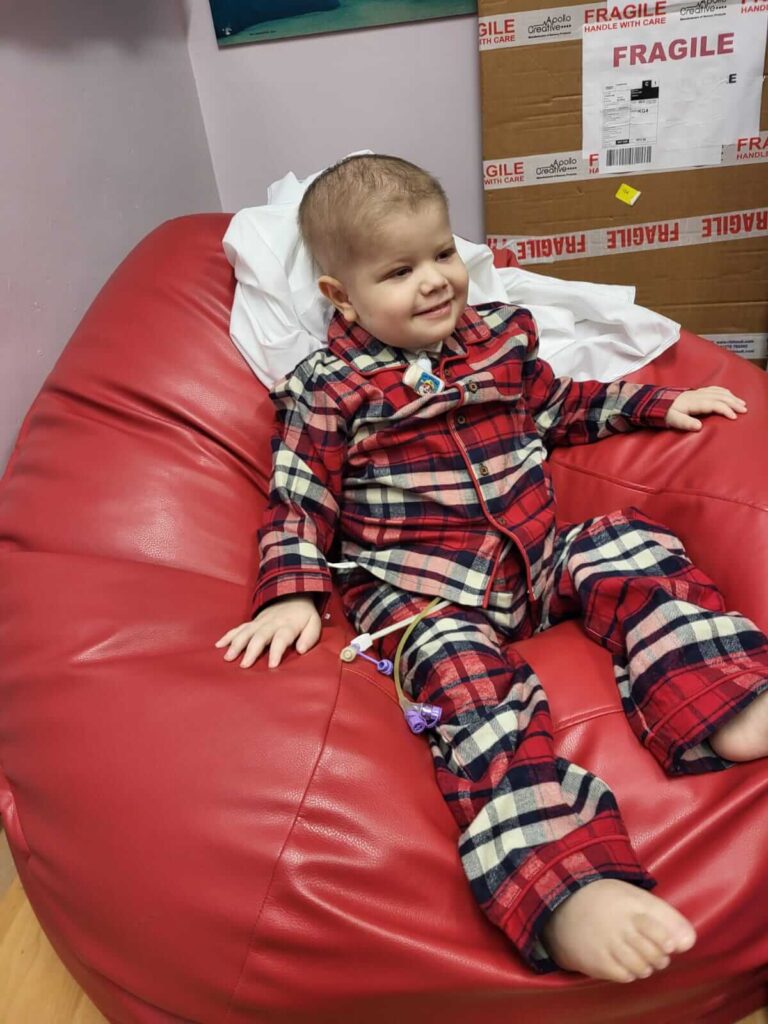
Suspected hernia
The Monday before Christmas 2021 a lump appeared on Archer’s left abdomen; I immediately thought the worst but everyone tried to convince me it was something like a hernia. On the Wednesday, I took him to the GP who couldn’t determine what the lump was and so sent off a two-week referral. Christmas was somewhat subdued whilst we waited for an appointment and Archer wasn’t as lively as we knew he could be. The Tuesday after Christmas, he was awake until the early hours of the morning in pain with his abdomen, so off to A&E we went. Whilst in A&E, increasingly senior members of staff would all come look at Archer and were unable to determine what the mass was; so it was decided to admit him to E17 as they believed it was located within the kidney area.
Neuroblastoma diagnosis
Within days, Archer had had ultrasounds and an MRI under general anaesthetic to try and identify what the mass was. Eventually, the surgeons came to see us to say that they wouldn’t be doing anything in the immediate future and to ask if oncology had come to speak to us, at that point it didn’t even occur to us what oncology was. When the oncology consultant came to talk to us, she used the word tumour, before cancer, but the diagnosis quickly dawned on us. He was sent on the emergency list to have a biopsy do and a Hickman line put in, as they were obviously concerned and were hoping to start treatment ASAP. They were initially unsure of whether Archer had Neuroblastoma or a Wilms tumour, so treatment was delayed whilst he underwent further testing to try and determine the diagnosis; however they eventually go to a point, whilst waiting on the results of an MIBG, to start treatment as if it was Neuroblastoma, they’d rather attack it head on and then pull back slightly, than not give high enough doses of chemotherapy.
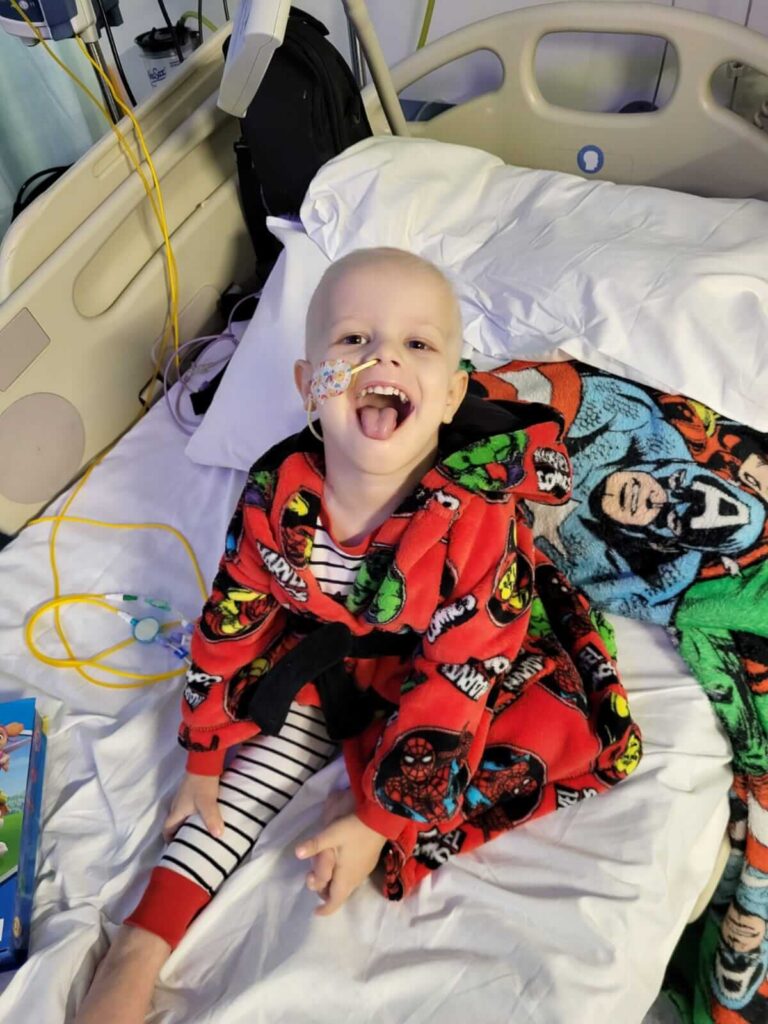

We made the decision to shave his head
On the 20 January 2022 we were admitted onto E39, we were told that usually the chemotherapy he was receiving would be given as a day case, however they wanted to keep an eye on him, so it would be at least one night on the ward, however it ended up being eight days before he was discharged due to them being unhappy with his heartrate and blood pressure. Archer was quickly identified as being particularly feisty and he spent a lot of time in the side rooms, simply because of how much he shouted and screamed, but that fight has served him well. Whilst at home we also made the decision to shave his head, as he had a full head of beautiful long blond hair, but we thought it would be less distressing to shave it than watch it all fall out. That moment was a real milestone and full in our face reminder that he had cancer, and we were about to start a long journey. Archer was then re-admitted two days later to start the next round of rapid COJEC, the chemotherapy for Neuroblastoma, and during that admission was when they confirmed that he had High Risk Metastatic Stage 4 Neuroblastoma, which had spread to his bone marrow, although luckily only by 5%.
Archer is feisty but that fight has served him well.
Severe side effects
Archer unfortunately seemed to get every side effect going, vomiting, severe mucositis, unable to stomach food, required oxygen on multiple occasions, he was bed bound due to how ill he felt. Due to Covid rules, only his dad and I were able to visit him, however as his third birthday rolled around they allowed his sister and grandparents to come and have a little birthday party. By this point his abdomen had started to swell, he was vomiting blood and his numbers weren’t great, but he was just being monitored. A few days after his birthday he had swelled so much, that he was struggling to breathe, and he was sent to ICU for the first time; we spent eight days in there during which he had an abdominal drain put in and was on a cpap mask until he was more stable and able to breathe with just a nasal cannula. We moved back to E39 on the 24 March, but on the 6 April he had an allergic reaction to platelets which resulted in him being sent back to PICU and being intubated for 24 hours.
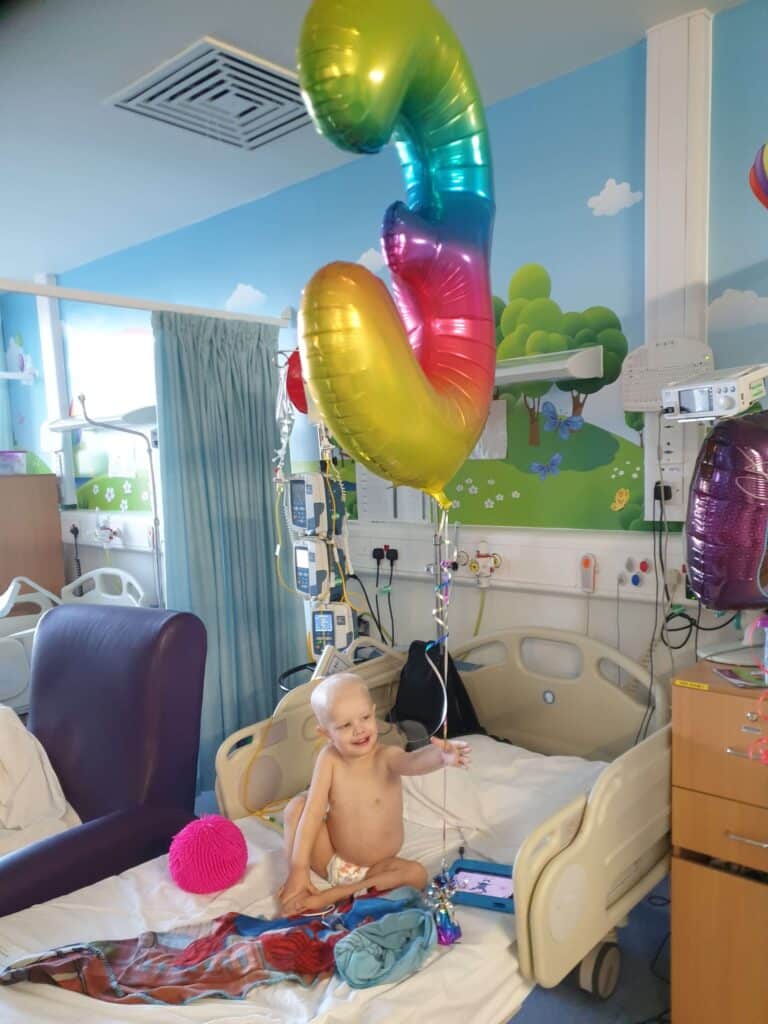

The stem cell harvest
Between his PICU stays, he had a third round of rapid COJEC and he was requiring near daily infusions of either platelets or bloods, which became a trend for him throughout treatment. Before our second trip to PICU it was decided to no longer continue with his current chemotherapy protocol and instead try second line chemotherapy, however he only got one round of this before his reaction and due to his health, it was decided to stop chemotherapy and reassess. Luckily scans and a bone marrow biopsy showed that his bone marrow was now clear, and his tumour had shrunk by around 75%. Due to complications with treatment and his inability to tolerate food, thus needing to be on TPN, he was unable to be discharged from the hospital until the 10 May. He had somewhat of a reprieve then from hospital stays, until he had to have his stem cell harvest; although he did require an overnight stay in between for a liver biopsy as they were concerned the cancer had spread. He coped with the stem cell harvest incredibly well and after a few days we managed to stay at home for around two weeks before going back to hospital for his high dose chemotherapy , 17 rounds of chemotherapy in six days, and then to have his stem cells transplanted. In those two weeks at home we managed to fit in a couple of family day trips, as we were unsure how long Archer would be in hospital for post high dose. He wouldn’t be discharged again until 22 December.
The worst time of our lives
We had been warned that he would be the sickest we had ever seen him after his high dose chemotherapy, PICU had already been prepared, but in typical Archer fashion he actually flew through it and although there were side effects, he coped with it a lot better than his previous chemotherapy. Unfortunately, due to continued feeding issues Archer wasn’t able to be discharged prior to his surgery on 18 August, however he was allowed two weeks of day leave in the run up which we were eternally grateful for, as the next few months ended up being some of the worst of our lives.
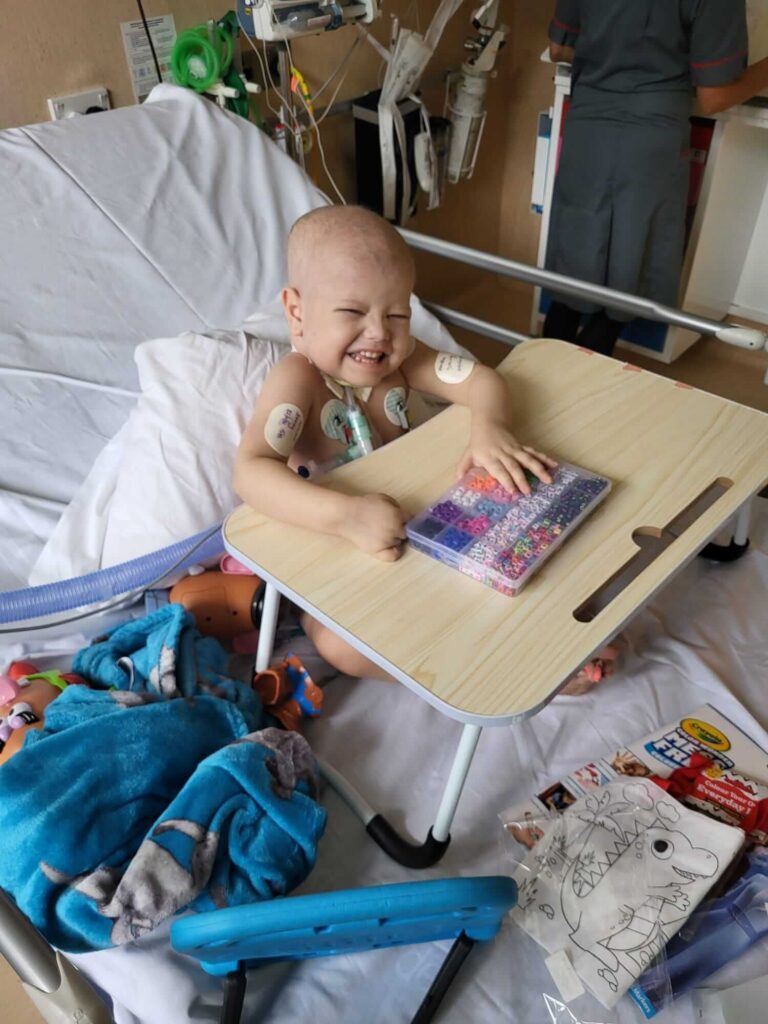
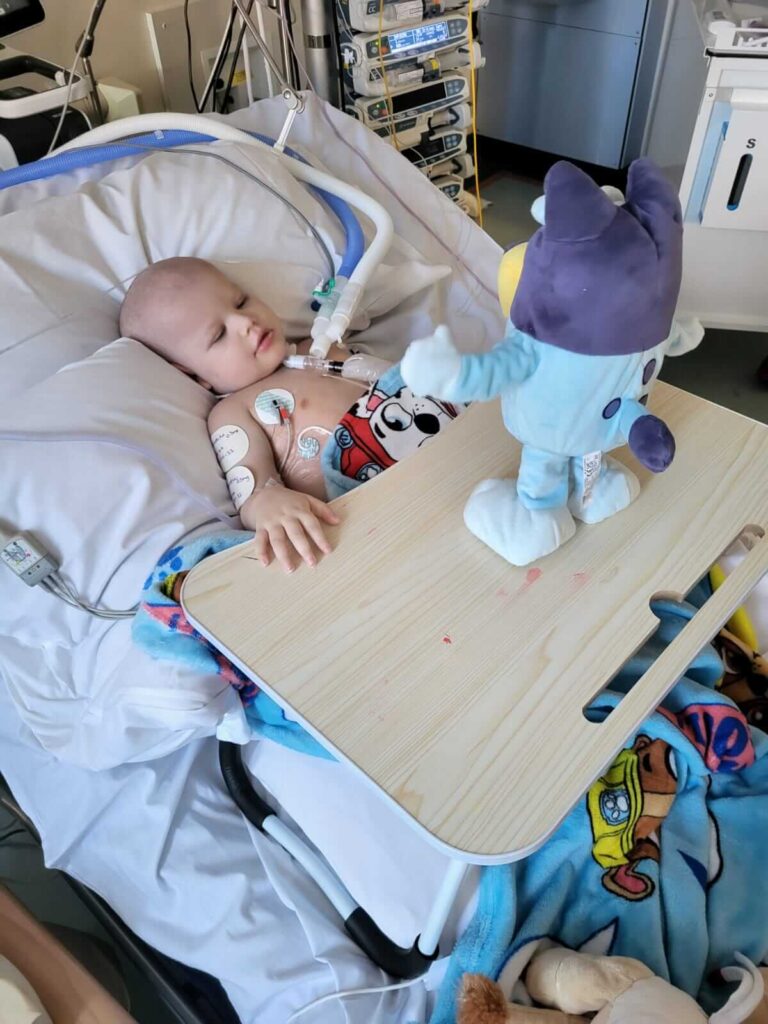
Surgery to remove the tumour
On August 18 Archer went in for his abdominal surgery to remove his tumour, his kidney and to have a peg-j inserted in hopes that that would work better for his feeding and medications as he was vomiting up or pulling out his NG tube out ever one to three days. I went down with him to the theatres at 9am and cuddled him whilst he was put to sleep and then started the anxious wait. At 4:30pm I got a call to say he was out of surgery and to go to PICU where the surgeon would meet us to explain what had happened. They managed to remove the entire tumour, alongside his dead kidney, however during surgery he lost all his circulatory blood which they replaced, and his lungs were struggling so he needed to remain intubated.
Intubation period
Archer was intubated for six weeks, during which he was on so many different combinations of sedatives, and they even brought in sedatives for ICU that they wouldn’t usually use in paediatrics as they were struggling to keep him sedated heavily enough; on multiple occasions he fought his sedation enough to throw toys at the consultants and to extubate himself. After six weeks, and a failed extubating due to withdrawals and his lung function, it was decided that he needed a tracheostomy. We were terrified that he wouldn’t survive the surgery given how poorly he was, but it was decided it was the only option; luckily the surgery was fairly straight forward, and we were able to start the process of weaning sedatives.
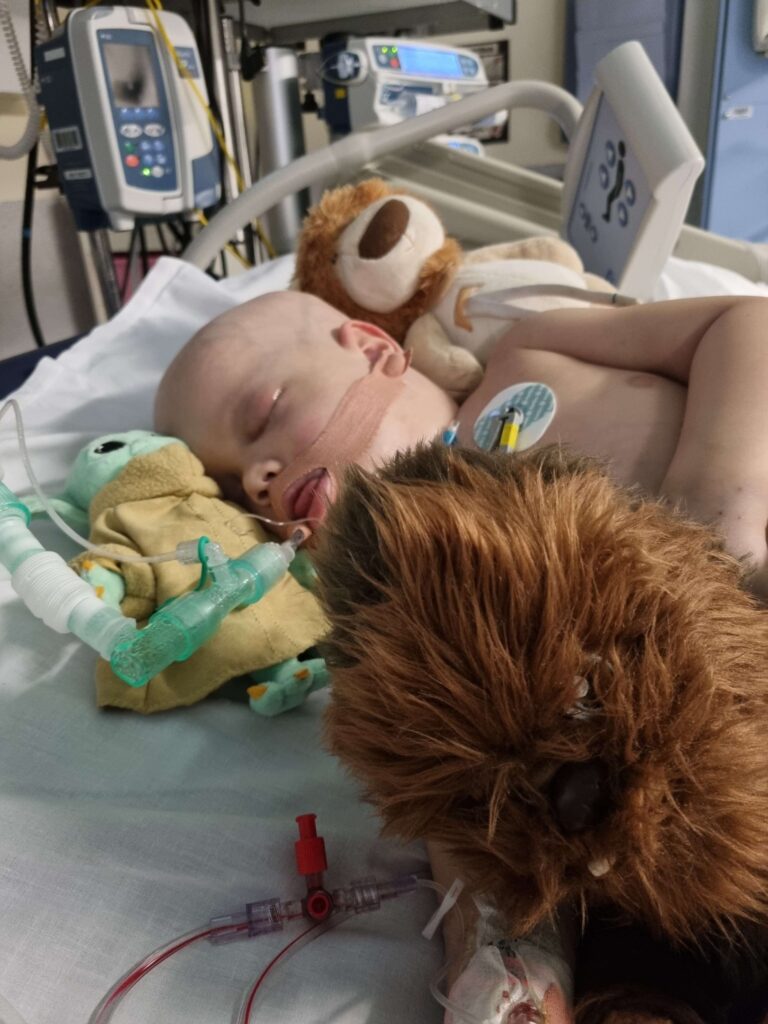
They estimated he would have two weeks
Within two weeks of having his tracheostomy he had a pulmonary embolism. I was trying to keep myself and him calm whilst he struggled to breathe due to the blood filling his lungs, even with 100% oxygen via the vent his oxygen reading was only 80%. He quickly deteriorated further, and we had a traumatic few hours where his section of PICU was cleared of all other patients and the majority of staff were working on his bed trying to keep him alive. His soon to be PICU consultant bagged him for over two hours to keep his lungs open enough whilst they came up with a plan, during which his oxygen levels were in the mid to late 50s. He was sedated again and put on an oscillator whilst we waited to see if he would pull through. We had a harrowing few days whilst we waited to see if he would improve, which he did, but eight days after his embolism he had an oxygen crisis, again he pulled through, but then another eight days later he had a second oxygen crisis. At this point we were taken into a room with his PICU consultant and one of the oncology consultants and told that there was nothing else they could do, and they would keep him as comfortable as possible whilst we waited, they estimated he would have two weeks.
They would keep him as comfortable as possible whilst we waited.
The steroids that changed everything
Having to tell his sister, whose birthday was just outside of the two-week timeline, was the hardest conversation we ever had to have. We continued to wean his sedatives so that we could spend time with him awake. For two weeks we worked with the best palliative care specialist to put plans in place for the time we had and for what we wanted once he passed. Archer, his dad and I and his grandparents all contracted COVID during this time, so the rules about who could visit him were constantly changing, but they did ensure at least one parent could stay with him. One night I had a conversation with one of the consultants about the options we had, we were advised what they thought would keep him most comfortable, with input from various teams, but ultimately the decision was up to us. We opted to try some steroids that would hopefully take the pressure off his lungs, and miraculously they turned everything around, no one involved in his care could believe it. Within two weeks of taking the steroids his oxygen requirements had dropped massively, he was awake and playing and laughing and none of us knew how to react.
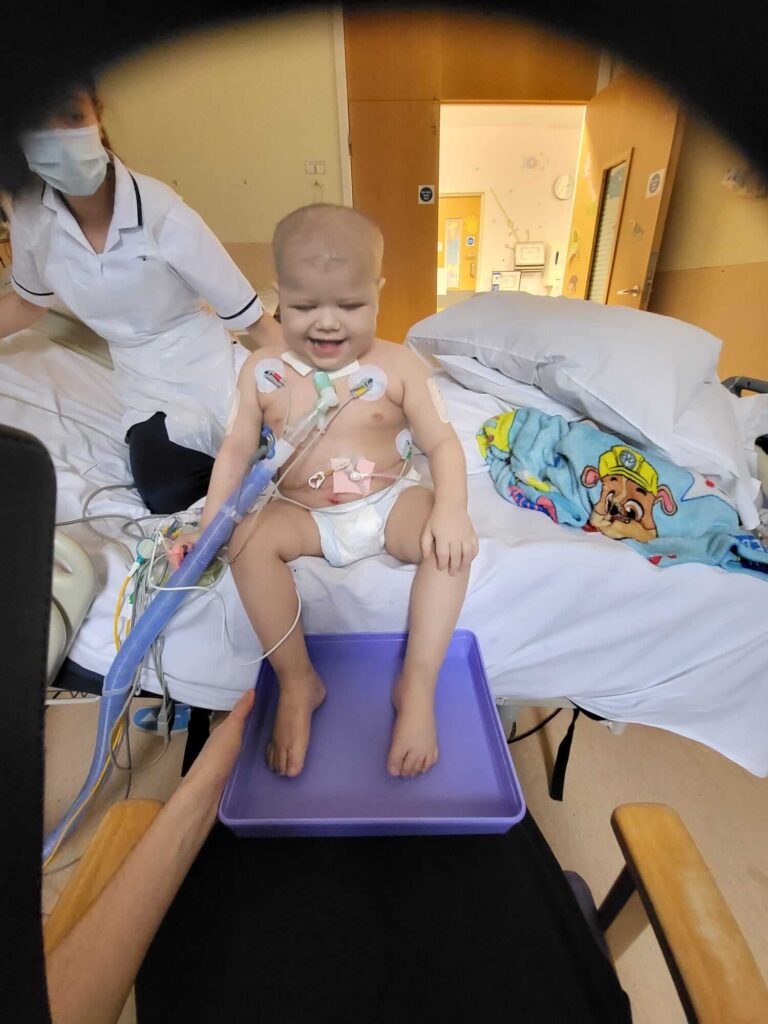
Making a recovery
By Aurora’s birthday, the 27 October, I got a message from Adam, as I was hosting her birthday, to say he was being moved to HDU. We stayed on HDU until the 22 December, during which we managed to get him off the vent completely, weaned most sedatives, got him out of bed for physiotherapy and even managed to take him down to the Christmas tree outside of hospital for him, alongside one of the other patients on HDU, to switch on the Christmas lights. We had a plan in place to get him home for a few hours Christmas Day, but instead he was discharged on the 22 as he had made such a incredible recovery that they didn’t think he needed hospitalisation.
He had made such a incredible recovery.
Archer is strong
Christmas was magical, simply because we didn’t think we would have it as a family. Since his discharge he has had a couple of hospitalisations for PEG replacements, due to contracting the flu and to have his Tracheostomy removed. He became a big brother on the 1 March 2023 and has adapted amazingly. Plans are in place for him to begin Reception in September and we have two caravan holidays planned so we can spend time as a family of five. Archer completed his cis-retinoic treatment at home, as he wasn’t allowed immunotherapy, and will finish radiotherapy on the 13 July, after 14 rounds, which has included daily general anaesthetics. We don’t know what the future holds, but this boy has fought tooth and nail to still be here and shown more strength and resilience than any person I know.
Jade, Archer’s mum, July 2023
We don’t know what the future holds.
How you can help
If you’ve been touched by Archer’s journey, help us invest in the high quality research that really matters which would otherwise go unfunded.
Have you or a family member been affected by childhood cancer?
Many of our supporters have been affected by childhood cancer – either through family, friends or their own personal experience. These patient stories can help inspire others to get involved with us, or can support our media work. If you have a story that you would like to tell,
Other stories
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.