Very bad news: alveolar rhabdomyosarcoma
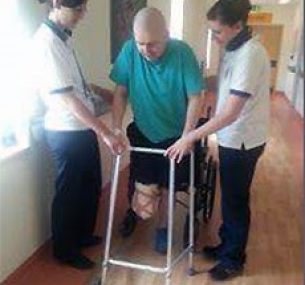
It was 2013 and I was 16. I had a very abnormal swelling on my leg that wouldn’t go away and was getting bigger and bigger. I eventually got a referral to see a specialist. I had a biopsy, an X-ray and an MRI scan. I got told very quickly that there was something very worrying going on and I was sent to see an oncologist.
I was given the very bad news that I had alveolar rhabdomyosarcoma, a rare type of soft tissue cancer. They needed to find out quickly if it had spread. I had a bone marrow biopsy, a bone scan, a CT scan and many blood tests. They found it hadn’t spread and was localised to the ankle bone area in my right foot.
They inserted a Hickman line for my chemotherapy regime. I was given Ifosfamide, Vincristine and Dactinimycin which involved two nights as an inpatient, followed by a 30-day break so that my blood count could recover.
The regime was pretty yucky and I threw up a lot. I was very tired for a few days but quickly recovered in each cycle.