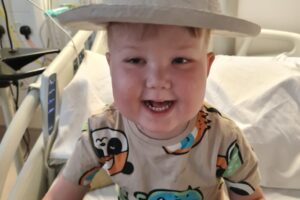
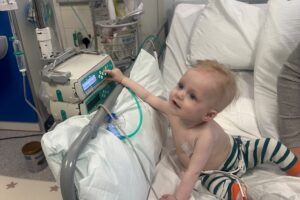
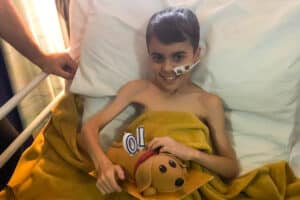
Chloe: “I felt dizzy, tired and pain in my abdomen”
Chloe was diagnosed with paraspinal neuroblastoma when she was 15 years old. Now in her 20s, Chloe shares her childhood cancer journey: Support children like Chloe so that they have a future they deserve.
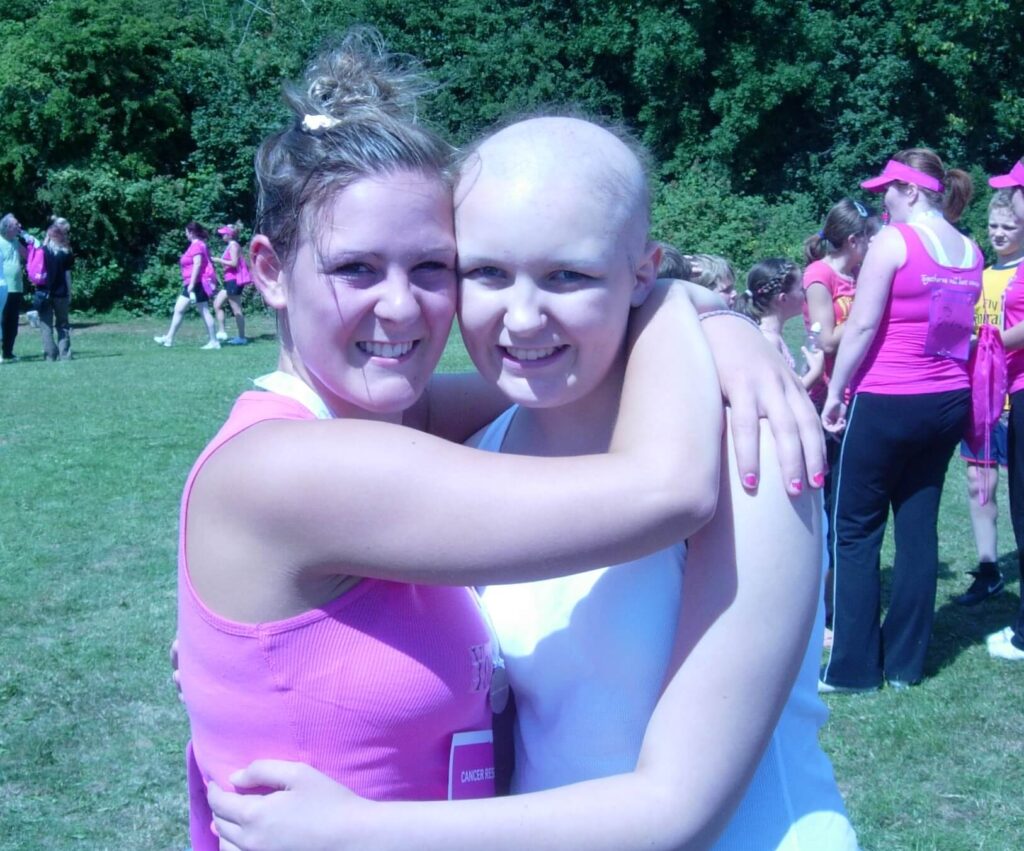
It started with non-specific symptoms
I had various non-specific symptoms for a while; fatigue, dizziness, nausea and pain, which was put down to chronic fatigue syndrome after numerous medical tests. However, during year 11 as I was preparing for my GCSE’s, I started experiencing an excruciating sharp pain on my left side of my back. I had an operation for a kidney issue three years prior so I assumed it must be kidney related, as the pain was the same side. I told my mum and this prompted us to book a GP appointment. During the appointment he palpated my abdomen and felt something unusual which unnerved me, but he reassured us something had probably moved during the kidney surgery.


They found a mass in my abdomen
I was referred for an ultrasound scan ‘just to be safe’. The doctors reaction meant both myself and my parents weren’t prepared for what was to come. A couple of weeks later my mum took me for the ultrasound scan. I laid on the bed and a warm jelly was put on my stomach and the scan started. The sonographer’s face changed. They had found a mass in my abdomen. At the time I was confused and not sure what a ‘mass’ was, but I could sense it was serious. We were told to see my GP that day and he said I needed to see a paediatrician urgently and looked into my eyes and said, “everything will be ok”. I thought to myself what does he mean by that? What is he too afraid to say?
It dawned on me that it was a cancer ward
The next day I carried on as normal and went to school; I found it difficult to concentrate as I was filled with dread. I was sitting in the school canteen on lunch break with my friends when I got a text message from my mum saying that I needed to go to the school reception, as we needed to go to the hospital urgently. I instantly felt an overwhelming fear, the knot in my stomach was getting tighter and tighter.
When my parents and I arrived at the hospital, we went onto a ward, we looked at each other with shocked expressions; the kids roaming the ward didn’t have hair. It dawned on me that it was a cancer ward…it hadn’t crossed my mind that it could be cancer and no one had warned us. Over a week I had numerous tests; a CT scan, biopsy of the mass, bone marrow aspirations and a MIBG scan.
We then got the devastating news that I had paraspinal neuroblastoma with adverse biology and it was stage 3. Due to my age and neuroblastoma being most common in under 5’s, the consultant had to consult other specialists to decide on a treatment protocol. It was decided that I would need the high-risk protocol, which included; chemotherapy, surgery, high dose chemotherapy and autologous stem cell rescue, radiotherapy and differentiation therapy.
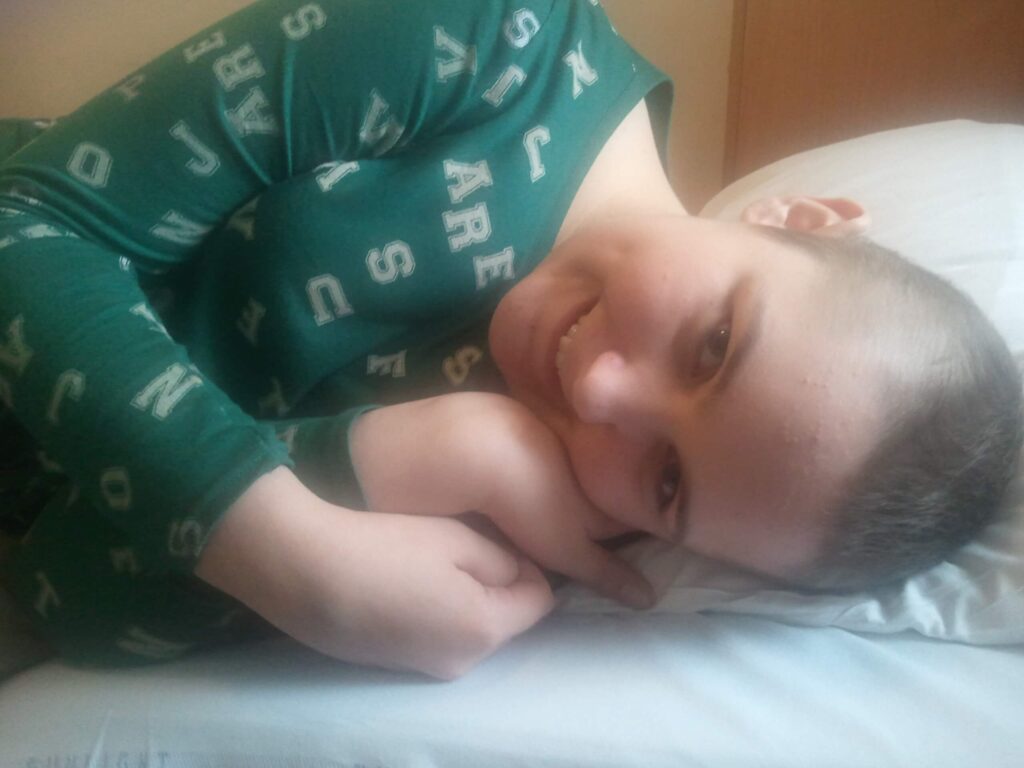

So the treatment journey begins
Before treatment started I had a portacath inserted and I had a short break from hospital. I then commenced induction chemotherapy (rapid COJEC). I was an inpatient for around three days and had seven days at home. I was to complete eight cycles. It was very intense; it made me very weak, I had low blood counts, nausea/vomiting and the worst part for me being a teenager was losing my hair. Around half way through induction chemotherapy I had a repeat CT scan to check the response. During cycle six, my oncologist came to tell us about the scan results…the tumour had not shrunk. They decided to bring the surgery forward, however the tumour was very close to nerve structures and was in my psoas muscle, so removing it all could have affected my ability to walk. I was terrified of the prospect of such major surgery. I had a two-week break to let my blood counts recover. I also had pre-operative assessment and an MRI scan to help the surgeon plan for my operation.
The day of my surgery
I had my surgery on 28 June 2010; my mum, dad and sister came to hospital on surgery day and had to wait an awfully long time worrying whilst I was in theatre. They only managed to remove around half of the tumour, as my leg moved when they tried to get a more extensive resection suggesting that the nerve root was contained in the tumour. I had mixed emotions I was worried that partial removal would affect my chance of survival, but I was so grateful that my ability to walk would not be affected. After a week in hospital recovering from surgery, I was finally discharged home. The pathology report of the tumour shown that although the tumour did not shrink it had worked to an extent, so I went on to have the final two cycles of chemotherapy I should have received.
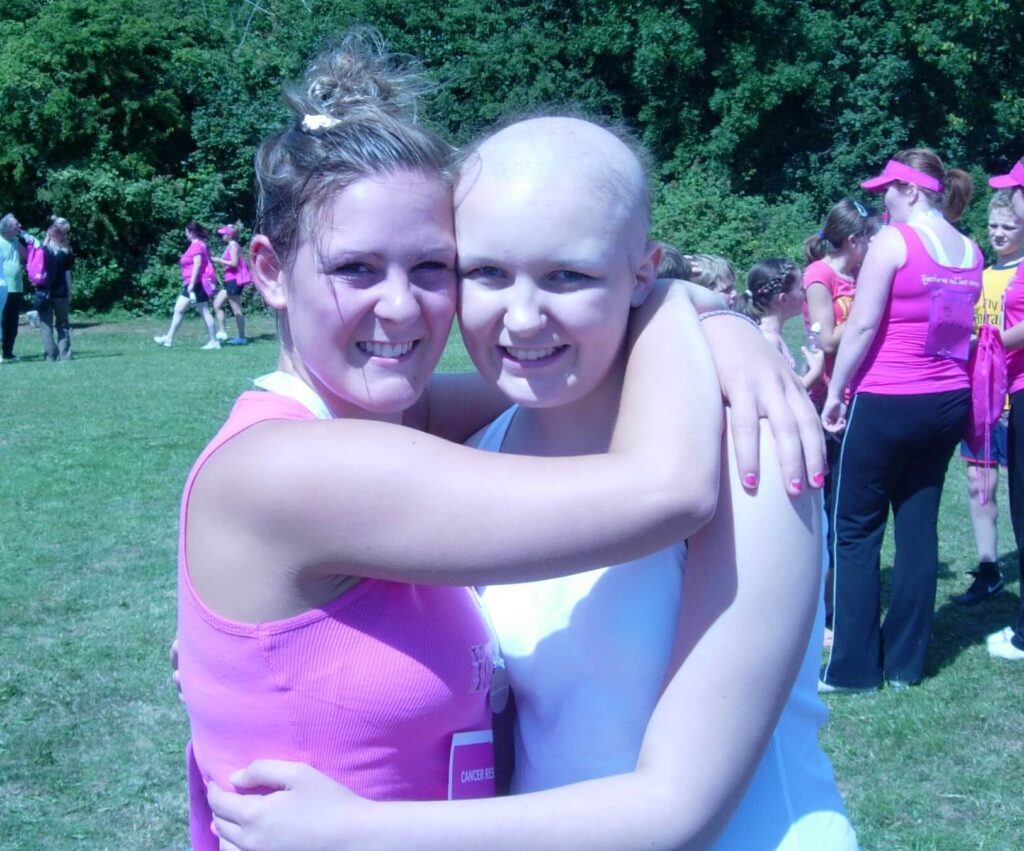
I went into isolation
Instead of having high dose chemotherapy, it was decided I would have MIBG therapy (a type of internal radiotherapy) along with chemotherapy, due to the fact my tumour did not respond to the induction chemotherapy. Before I could have the treatment, I had a vascath line inserted into my femoral artery in order to harvest my stem cells. I had two cycles of MIBG therapy; each one involved a week stay in a lead lined room with limited contact from others, as I was highly radioactive. It was incredibly isolating and I couldn’t have any home comforts, everything that went in couldn’t come out, as it would be contaminated with radiation. I had disease reassessment scans and the tumour had shrunk by a third, this was amazing to hear.
It was incredibly isolating and I couldn’t have any home comforts
The tumour had shrunk a little bit more
I went on to have 22 sessions of conventional external beam radiation. Eventually I was on the last stage of treatment, which was differentiation therapy, which involved taking 13-cis-retinoic acid; an oral medication. I experienced extreme side effects during the first cycle; I was admitted to hospital with severe migraines and vomiting, so the medication was reduced by 25%. The following cycles I tolerated better, however it still made me feel really unwell and I felt increasingly anxious. Due to the way it made me feel I stopped the medication slightly early. I had end of treatment scans and the tumour had shrunk a little bit more and was roughly the size of a tennis ball, but it was more of a stretched tennis ball! Both my parents and myself were apprehensive about there still being residual tumour, but we were reassured it would be monitored. I had my portacath removed and tried to move on and look forward. I had three monthly MRI scans for the first year, six monthly MRI scans for two years and yearly MRI scans for one year, which all shown stable disease.


The whole process was mentally and physically tough
I found the treatment extremely tough not just physically but also mentally. As a teenager my care free life was taken away. I suddenly had to undergo all these gruelling treatments, to give me a chance of a future. I met friends along the way whom of which I made bonds with; one was a lad who I met when I had radiotherapy and another was a young girl of a similar age with the same cancer we spoke daily. They unfortunately both died and this resulted in me having survivor’s guilt. When I finished treatment I had all these intense overwhelming emotions, I expected to just be so happy I had finished treatment, but instead I felt like a shell of my former self and incredibly anxious. It was like I did not know how to live a normal life anymore. It wasn’t as easy as picking up where I left off; I had changed and was still living through the trauma of going through cancer.
Long term side effects
During my treatment I started getting menopausal symptoms and after tests, it was confirmed to be ovarian failure at 16 years old, so I am now on hormone replacement therapy. I also have chronic nerve pain, which at times has been difficult to control.
I now live with long terms effects caused by the tumour and the treatment

I’m now a qualified children’s nurse
Despite this I went full steam ahead I continued my A-levels and I applied to university to study children’s nursing. My experience with cancer really influenced my decision to pursue a career in nursing and knew it was the right path to take. I got into university and completed my three year course; qualifying as a paediatric nurse in the summer of 2016. I started my first job as a qualified paediatric nurse on a children’s medical ward, caring for both acute and chronically ill children. The whole process has really helped me grow in confidence and skill. It is such a privilege to be able to treat and care for ill children and their families. I truly feel that no matter how hard my journey was, it has shaped me as a person and it has taught me to live in the moment and treasure those little things in life. I am very lucky that my family have been with me every step of the way and gave me the confidence to achieve my dreams.
I published a book
More recently I published a book called ‘Beyond Fear is Hope’, which details my cancer journey and life beyond cancer. It really expresses the intense emotions I had during diagnosis, treatment and also life after treatment. When I finished my treatment, I felt really lost and just blocked out the trauma. I felt like this was the ‘wrong’ way to feel and I should have nothing but gratitude. But now I have discovered that it was not the wrong way to feel and want to get my story out there to help other young people going through cancer. I also want to get the awareness out there of the challenges faced going through such adversity. There is a special section at the end especially for young people with cancer with my top tips in a ‘things I wish I had known’ perspective. Every experience, however hard or painful, is a part of your story, and not something you can erase.

How you can help
If you’ve been touched by Chloe’s journey, help us invest in the high quality research that really matters which would otherwise go unfunded.
Have you or a family member been affected by childhood cancer?
Many of our supporters have been affected by childhood cancer – either through family, friends or their own personal experience. These patient stories can help inspire others to get involved with us, or can support our media work. If you have a story that you would like to tell,
Other stories
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.