Understanding cancer
Acute Lymphoblastic Leukaemia (ALL)
Acute lymphoblastic leukaemia is a type of childhood leukaemia that affects the white blood cells, which are vital for fighting infections in children. Understanding acute lymphoblastic leukaemia survival rate and treatment options can help families navigate a diagnosis and access the right support.
What is Acute Lymphoblastic Leukaemia?
Acute Lymphoblastic Leukaemia is a type of Leukaemia, a cancer of the white blood cells. Your child’s body needs white blood cells help to fight infections.
There are two different types of white blood cells – lymphoid cells (also known as lymphocytes) and myeloid cells. Normally these cells, which are produced in the bone marrow, repair and reproduce themselves in an orderly and controlled way. In leukaemia, however, the process gets out of control and the cells continue to divide but do not mature.
Acute Lymphoblastic Leukaemia, which is often called ALL, is an overproduction of immature lymphoid cells, this is when white blood cells that have not fully developed before being released from the bone marrow into the blood, called lymphoblasts or blast cells. Immature lymphoid cells fill up the bone marrow and stop it making healthy blood cells. As these cells are immature, they cannot work properly. This puts you at increased risk of infections. Symptoms of leukaemia in children such as bruising, and anaemia are caused by the bone marrow’s inability to make enough healthy red blood cells and platelets.
What are the symptoms of ALL?
Childhood leukaemia develops quickly. It’s possible for some or all of these symptoms of leukaemia in children to be apparent.
Signs and symptoms of ALL in children and babies can include:
- frequent and persistent infections
- unusual bruising
- breathlessness and coughing
- paleness
- unusual bleeding
- tiredness
- anaemia
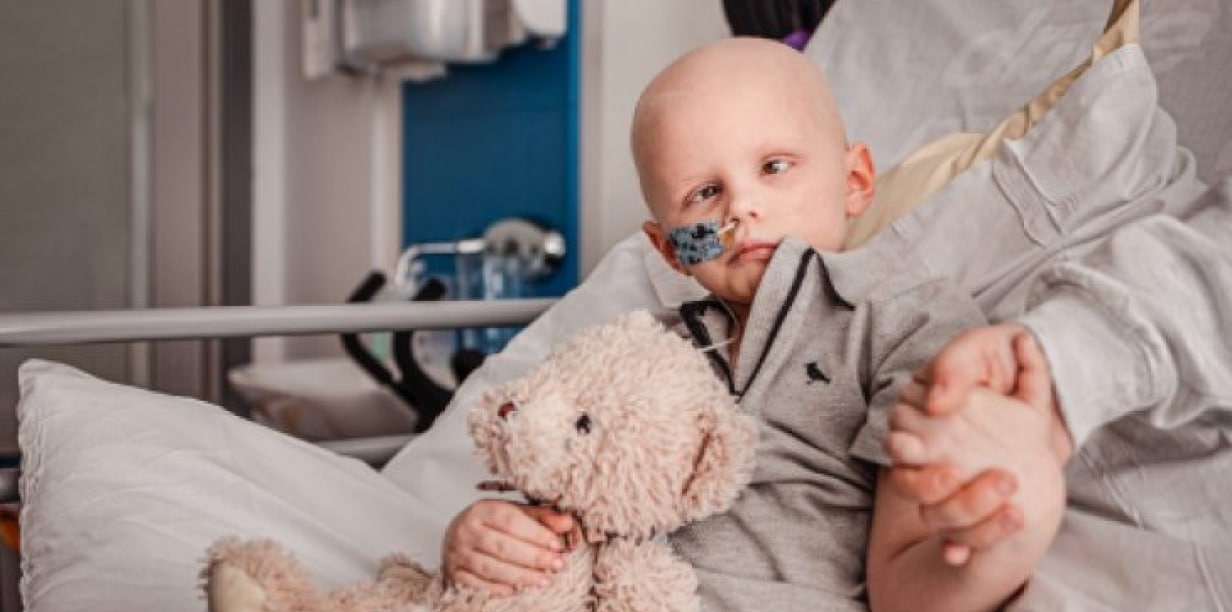
Learn about a real-life story of ALL with Isla-Mae, including her early symptoms of this type of leukaemia and diagnosis.
Incidence
Leukaemia is the most common childhood cancer, accounting for nearly a third of all cases (31% and 29% in boys and girls, respectively) in Great Britain. ALL accounts for around four-fifths (78%) of all leukaemias diagnosed in children in the UK.
There is a peak in incidence of Acute Lymphoblastic Leukaemia in children aged two to three years; more than half of all children diagnosed with Acute Lymphoblastic Leukaemia are under the age of five years.
Boys have a greater risk than girls of developing ALL, by a factor of 4:3. The reason for this difference between the sexes is not known. Boys also require a longer duration of treatment.Below you will find information about the different types of cancer which can affect children, teenagers and young adults.
Diagnosis
What would you expect to happen first, when you see your GP?
Once this has happened and the doctors have the results, you will be referred to hospital for further tests. A sample of bone marrow will be taken to confirm the exact diagnosis.
A diagnosis of childhood leukaemia is usually made on the basis of a blood test. This test will reveal low numbers of normal white blood cells and large numbers of abnormal white blood cells.
How is ALL treated?
What would you expect to happen during treatment?
Whilst over 90% of Acute Lymphoblastic childhood leukaemia cases can now be successfully treated (with survival for 5 years or more), treatment is long and gruelling, lasting two years for girls and three years for boys.
The initial aim of treatment is to achieve a state called remission where most of the leukaemia cells have been killed, allowing the production of normal blood cells to resume. This stage involves the use of several drugs in combination and usually lasts between three and eight weeks, depending on how quickly you respond to treatment.
Following this initial or induction treatment there will be further blocks of consolidation treatments followed by maintenance chemotherapy which can last up to three years. As well as chemotherapy, some high-risk children may also require and/or a stem cell (bone marrow) transplant.
The initial aim of treatment is to achieve a state called remission where most of the leukaemic cells have been killed, allowing production of normal blood cells to resume. This stage involves the use of several drugs in combination and usually lasts between three and eight weeks, depending how quickly the child responds to treatment.
Almost all children will have leukaemic cells remaining when they achieve remission. This is known as minimal residual disease or MRD. It is necessary to give further blocks of treatment to eradicate the disease completely and achieve a cure. Standard consolidation therapy involves two blocks of chemotherapy at intervals of roughly four and eight months from diagnosis but protocols vary according to a number of factors including MRD status. For high-risk children, treatment may be intensified by the inclusion of additional blocks of treatment, or by the inclusion of additional drugs in the periods of maintenance therapy between the intensification blocks. Intervals of time are left between blocks of treatment in order to allow the child’s body to recover and to minimise the risk of treatment-related complications.
Some leukaemic cells may cross the barrier into the fluid which surrounds the brain and spinal cord. The chemotherapy drugs do not penetrate this barrier very well, so it is necessary to inject the drugs directly into the fluid. This is known as an intrathecal injection. Occasionally radiotherapy may also be used to target the CNS.
Children with ALL require a phase of extended ‘maintenance’ therapy to prevent relapse. This involves taking daily tablets and having monthly injections of chemotherapy drugs. Maintenance therapy takes the total duration of treatment to two years for girls and three years for boys. This stage of treatment is carried out on an outpatient basis, usually on a ‘shared care’ basis between the specialist centre and the child’s local hospital. Children will usually be well enough to resume most of their normal activities and return to school. They will be closely monitored during this stage.
Transplantation is not routinely used in the treatment of children with ALL cancer. It is only used in certain high-risk groups – in children who have relapsed early in their treatment or who have experienced more than one relapse.
Radiotherapy is not routinely used in the treatment of childhood acute lymphoblastic leukaemia. Children who are found to have leukaemic cells in their brain and spinal fluid when they are diagnosed may need radiotherapy. In some situations, it may be necessary for boys to have radiotherapy to their testicles since leukaemic cells can survive in the testicles despite chemotherapy.
Following completion of treatment, all children will continue to be monitored for symptoms of both disease relapse and treatment complications. Checks will take place every two or three months for the first year, gradually becoming less frequent.
What is happening in the body and are there any side effects?
The treatments used in childhood ALL often cause side effects. Most side effects are temporary and can be minimised with good supportive care. The most common short term effects include:
- nausea and vomiting
- hair loss
- reduced resistance to infection
- bruising and bleeding
- tiredness
- diarrhoea
A number of children may develop persistent side effects as a result of treatment, sometimes many years later, these are known as late effects. These can include:
- reduced bone growth
- reduced fertility
- changes in heart function
- slightly increased risk of developing a second cancer later in life
Follow-up and Acute Lymphoblastic Leukaemia relapse
All children will be followed-up at regular intervals after their treatment for ALL to monitor their progress and check for treatment-related problems.
Although most children with ALL will achieve remission, up to a quarter of these children will relapse – their disease will return. Most relapses occur within three years of treatment ending.
Relapsed ALL tends to be more resistant to treatment but many children can be successfully re-treated.
A stem cell transplant may be an option for some children who relapse early in treatment or who experience more than one relapse.
The likelihood of a relapse progressively decreases with time, particularly once maintenance treatment is completed.
Survival rate
How effective are the treatments – What are the survival rates?
The survival rate is highest in children diagnosed after one year of age. Until the 1960s, childhood leukaemia was incurable. Today, thanks to improvements in care and sustained investment in research, the outlook for young patients diagnosed with ALL has dramatically improved.
Can it come back?
The likelihood of a relapse progressively decreases with time, particularly once maintenance treatment is completed.
When he was 3 years old, Benji began to get leg pain at night and was later diagnosed with ALL. Having recovered from treatment, Benji is now 12 years old. Read Benji’s story.
Research
Most children have their treatment as part of a clinical trial. These aim to improve understanding of the best way to treat the childhood leukaemia, usually by comparing the standard treatment with a new or modified version. The dramatic improvement in ALL survival rate has been brought about by a continuous series of clinical trials which have pioneered new ways of treating the disease.
Understanding the types of childhood cancer
Each type of childhood cancer has unique characteristics and treatment needs. Here, we provide an overview of the 10 primary types to help you learn more about the various diagnoses that impact young lives.
Topics on this page
Related topics
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.

Kaiden’s Medulloblastoma Story
Kaiden’s Medulloblastoma Story “I have huge hopes that one day in the future, children like Kaiden can have much kinder…
Read more Kaiden’s Medulloblastoma Story
Too Big Campaign – Press Release
‘2 BIG’: OVERSIZED EVERTON KIT HIGHLIGHTS HARSH REALITY OF CHILDREN RECEIVING ADULT CANCER TREATMENT 11-year-old Kaiden Edwards, who is living…
Read more Too Big Campaign – Press Release
Fundraiser of the Month: Izzy
Fundraiser of the Month: Izzy Our Fundraiser of the Month for April 2026 goes to the amazing Izzy, who set…
Read more Fundraiser of the Month: Izzy
Teenage and Young Adult Cancer Awareness Month 2026
Childhood cancer survivor shares his story for Teenage and Young Adult Cancer Awareness Month after completing a marathon and inspiring others to follow.
Read more Teenage and Young Adult Cancer Awareness Month 2026
Alfie’s Glioblastoma Story
Alfie’s Glioblastoma Story Alfie was only 3 months old when his dad noticed something wasn’t right. Read his full story…
Read more Alfie’s Glioblastoma Story
Teddy’s Leukaemia Story
Teddy’s Leukaemia Story Teddy was only 3 when he was diagnosed with Leukaemia. His father, Sam is sharing Teddy’s story…
Read more Teddy’s Leukaemia Story
2026 Research Grant Call launched
Children with Cancer UK launches the 2026 Research Grant Call to accelerate breakthroughs in childhood cancer
Read more 2026 Research Grant Call launched
Emil’s Brain Tumour Story
Emil’s Brain Tumour Story Hear Emil tell his story of his brain tumour diagnosis when he was 9 and how…
Read more Emil’s Brain Tumour Story
Ren’s Neuroblastoma Story
Ren’s Neuroblastoma Story Ren was diagnosed with Neuroblastoma at just eight months old. His mum Harriot is sharing his story….
Read more Ren’s Neuroblastoma Story
Brain Tumour Awareness Month
Children with Cancer UK is raising awareness & funding new research to deliver more targeted treatment for children with brain tumours
Read more Brain Tumour Awareness Month