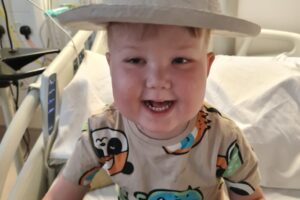
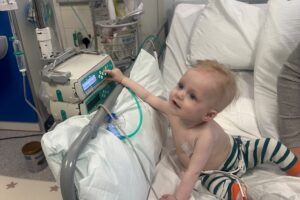
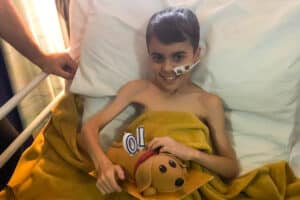
Orla’s medulloblastoma brain tumour story
Orla was diagnosed with medulloblastoma, a type of brain tumour in September 2022 when she was just one years old. Tragically, Orla did not survive her diagnosis and passed away on 12 August 2023. Her mum Naomi shares their story: Support children like Orla so that they have a future they deserve.
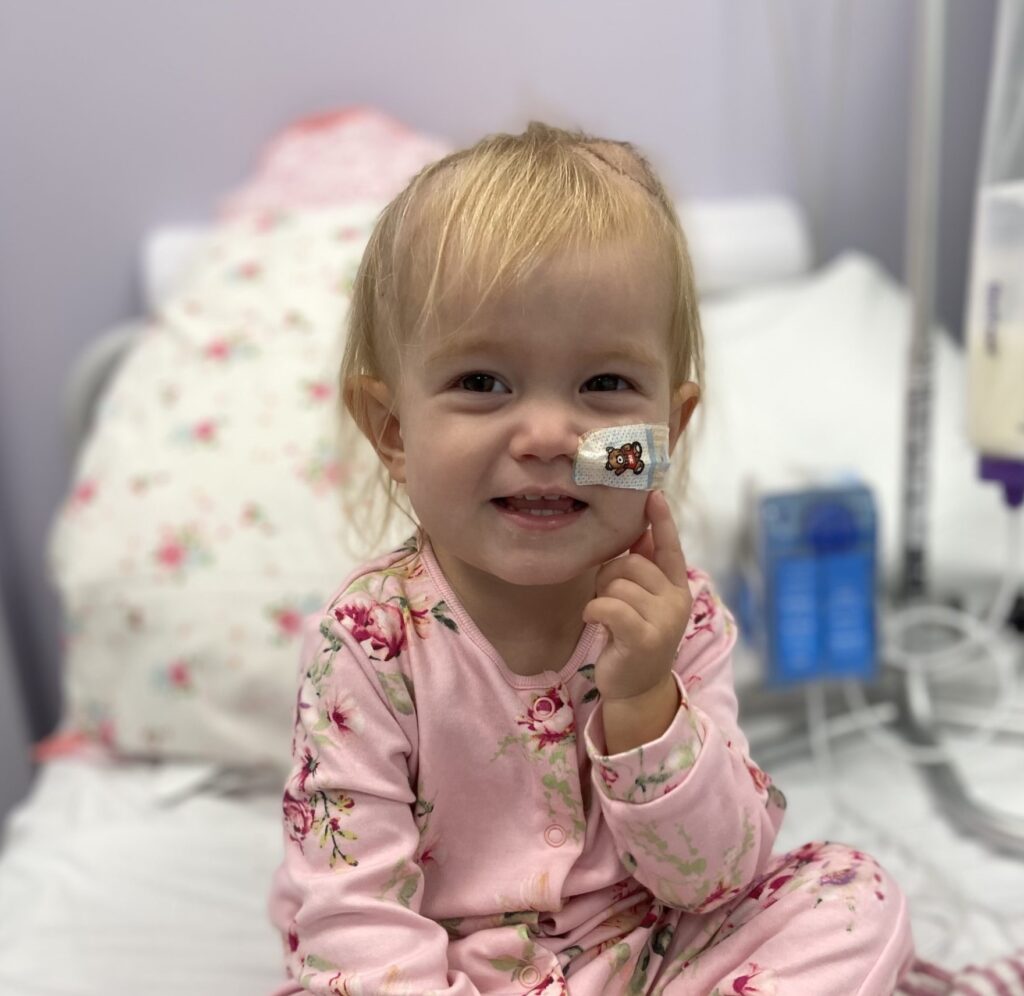
She’d always been on reflux medication
In August 2022, my husband Adam and I were on a family holiday with our three girls. Orla had been on reflux medication since she was a baby, but we knew she needed weaning off them at some point. Being out of routine on holiday, it happened naturally, and she was fine, running around and having fun. We were back home about a week, when one morning I found a patch of yellow sick in her cot. She seemed a little off that day and was sick again and we thought maybe it was withdrawals from the reflux meds. Then she started being a bit off-balance when she was walking, so I took her to the GP. I thought maybe she was just weak from the sickness, and not eating well. The doctor sent her for blood tests which came back clear.
She was being sick all the time
I was still concerned so I made an appointment for Orla to see a paediatrician privately, the same person she saw as a baby with her reflux problems. But before that appointment she was being sick more frequently and one evening in early September it was really nasty so we took her to A&E. They checked her over but couldn’t find anything wrong. She continued with constant sickness and became really lethargic, and clingy. On 15 September we saw the private paediatrician. Typically, Orla was really well that day, and we thought we looked a bit silly for being so worried, but he arranged for more specific bloods to be taken the following week, thinking she may be gluten intolerant. The day we had bloods we ended up taking Orla to straight round to A&E again, because she couldn’t stop being sick and she’d lost so much weight. We were so worried about her; she was so weak and it was incredibly frustrating that nobody could tell us what was wrong. The hospital ended up admitting her and she was there for 10 days, getting progressively worse. They put a gastric tube into her stomach through her nose to feed her, because she wouldn’t even drink water or take any oral medication.
We’re going to get Orla through this
To our relief she managed to take some milk one night and we thought she was doing better, but then she projectile vomited it all back up. It just kept coming and coming, and it was terrifying to see. The doctors thought she had a gut motility problem and were in talks with the hospital to see a specialist gastroenterologist and get her transferred. We were waiting for a bed to become available there, when on 29 September she had an ECG and an echocardiogram because her heart rate was low and her blood pressure was high. They also did a CT scan, because that combination indicated possible cranial pressure. Later that afternoon a specialist nurse came to me and asked to speak to me and Adam. I looked at her and I just knew something was really wrong. She took my hand and said ‘it’s OK we’re going to get Orla through this’.

It felt like the whole world was crashing down around us
We were taken to an empty ward; two specialist nurses, a paediatric consultant and the doctor who was looking after Orla sat us down. They said ‘we’ve found a mass, and fluid, on Orla’s brain’. I just burst into tears and Adam dropped to his knees in disbelief; we couldn’t believe this was happening to our baby. It felt like the whole world was crashing down around us. I can’t even remember what else was said because the whole thing felt like an out-of-body experience, other than we needed to get her transferred to a major children’s hospital immediately. They said ‘you don’t need to do anything, when you get there everyone will be there for you’. We arrived a few hours later and were taken straight to the children’s ward where the surgeons and anaesthetists were waiting for us.
Operating on the tumour
The first thing they wanted to do was fit Orla with an external ventricular drain (EVD) to remove the excess fluid from her brain and relieve the pressure. I remember so many forms with all these awful risks listed that we needed to sign. Adam asked what our other options were, but the surgeon just said there are no options, she had to have this done. It was awful; we had no control of anything that was happening to our baby, and we had no way of helping her. We had to just wait and hope. They operated at about 10:30pm and we got a call after 1am to say she was out of theatre and it had gone well. Her tumour was a solid mass, but it also had a cyst attached to it, which they managed to drain too. It went from being 7cm in total to about 4cm. The next morning, she was really groggy but the following day she woke up and it was literally like having our old Orla back. She was happy; she wanted to eat and play and wasn’t being sick. It was so amazing to see, and for a few days we were all happy.
Receiving the diagnosis of high-grade medulloblastoma
They performed the tumour resection on 4 October, and we were told it would take about 10 hours, so Adam’s brother and a couple of his close friends came to London to meet up with us for lunch to help distract us. Adam and I ended up going shopping in Oxford Street because we only had a few clothes with us, not having expected to be at the hospital for so long. We bought Orla a load of Frozen toys from the Disney Store too. It was so strange; it was really busy but to us it felt quiet and eerie. It was like we weren’t fully there; we were just floating through the crowds. We went back to wait for Orla to come round from the operation, but she was in a lot of pain when she did. It was heart-breaking seeing her in so much distress. She wouldn’t settle and the anaesthetist had to stay with us for hours and give extra pushes on the morphine pump to calm her down. The surgery was a success, they managed to remove the whole tumour. But there were side effects; she developed Posterior Fossa Syndrome and couldn’t swallow. She kept choking and we had to work with speech therapy to help her eat and drink safely again. She had a bit of paralysis down one side of her face too and couldn’t walk, so she needed physiotherapy. But we accepted all that, hoping we were nearing the end of this gut-wrenching experience. But then a few days later we were called in because they had the results of her biopsy. Of course we were hoping it would be low grade, but we found out it was a high grade medulloblastoma. They said it looked typical for this tumour in a child under three, which meant she would be low risk within her group, but they still needed the molecular results back. Those would take up to six weeks, but they didn’t expect to see anything out of the ordinary as it would be incredibly rare. It was as favourable and positive as it could be, but we were still being told our little girl had cancer. I couldn’t really process it and Adam was really upset, he couldn’t talk. His mum was also battling ovarian cancer, and having his mum and our daughter deal with cancer at the same time was devastating. Nobody should have to deal with that much trauma in one go. We left GOSH on 18 October with a plan to start chemotherapy the following week.
High-Risk Protocol
On 25 October we all went up on the first day of treatment as a family, Adam took the girls into London and I stayed with Orla. But nobody came to take her and nothing was happening. I asked what was going on and her specialist oncologist came in and said we needed to talk about Orla’s treatment. I knew it wasn’t good news from the look on her face. She said we needed to change Orla’s treatment plan because the molecular results had already come through. Orla had a MYCN amplification in the tumour but didn’t have the TP53 mutation; normally they are seen together. I said what does that even mean? But she didn’t know, so they moved Orla to the high-risk protocol. Again, everything came crashing down around us. It felt like every possible bit of bad news we could get, no matter how unlikely, we were getting. It meant Orla couldn’t start treatment and we had to go home. Adam was also really angry that they’d told me all this on my own, and everything was so unclear.

Ovarian Cryopreservation
On 28 October we went back to GOSH and Orla started her induction chemotherapy, with five cycles. She did well on her first cycle, and we were able to take her home, but then she spiked a temperature, and we ended up back at hospital for over a week. Then she got an infection and mucositis, so she needed a peg to be fitted into her stomach to feed her as it was too painful putting a tube down her throat. At that point she was offered ovarian cryopreservation, where they would freeze Orla’s tissue for use in the future, because it was likely the chemotherapy would make her infertile. We were told it was quite new for a child this young to be offered this procedure on the NHS. We read up about it and went ahead because we wanted Orla to have the opportunity to make her own choices. So, on 25 November we went to a specialist hospital in London to have the cryopreservation and the peg fitted at the same time. Later that day we went for the second round of chemotherapy but Orla developed a respiratory virus. She was so unwell; she wasn’t tolerating any feeds and she did cycles two and three without going home in between. They also harvested and froze her stem cells ready for them to be given back to her after high-dose chemotherapy. She didn’t leave hospital until 10 January 2023.
During that time Adam’s mum, Gill, also deteriorated. It was a real challenge, Adam was visiting her every day in a hospice, was seeing Orla at GOSH and trying to see our other two girls was well. We sometimes had to get friends to look after the Ava and Poppy, and they started struggling too, sometimes I didn’t see them for a week. Gill ended up leaving UCLH at the beginning of November, because there was no more treatment they could give her. She passed away at the beginning of December 2022. It was a truly awful time.
They couldn’t find a single case like Orla’s
We did everything we could to make Christmas as magical as we could for the girls. We had to spend it at GOSH, but the Young Lives vs Cancer charity arranged accommodation so we could be up there all together as a family. On 16 January 2023, Orla went back in for the fourth chemotherapy cycle, and they had to change one of the drugs because it was damaging her high-frequency hearing, resulting in partial hearing loss. We were due to do cycle five in February, but they skipped it, because of concerns over the MYCN amplification and what it means for her tumour. Her consultant was working with other specialists to try to find out if anybody else in the UK or Europe has this tumour with the same amplification, without the TP53 mutation. They couldn’t find a single case. Because of that they didn’t know whether they were over or under treating it. Her consultant chose not to expose Orla to any more toxicity from the induction chemotherapy. Instead, the specialists agreed to start her on the high-dose chemotherapy on 20 February, which she had to have because she was too young for radiotherapy. It involved a really high dosage over about six days, which wiped out her bone marrow and she needed her stem cells returned to her straight after. They estimated wanting to keep her in hospital for about eight weeks for recovery, and because she was immunocompromised, so there was a really high risk of infection.
She did amazingly well during the chemotherapy. She had hardly any side effects, unlike before. All the medical staff said she was doing incredibly well. After about five weeks the only thing really keeping us in the hospital was to re-establish Orla’s feeding, and we were told if that was sorted, we could be going home by the end of the week. She’d had to be on gut rest for a while, and was being fed via a Hickman line, but was gradually having more time off the machines, and was being fed primarily via a line at night.
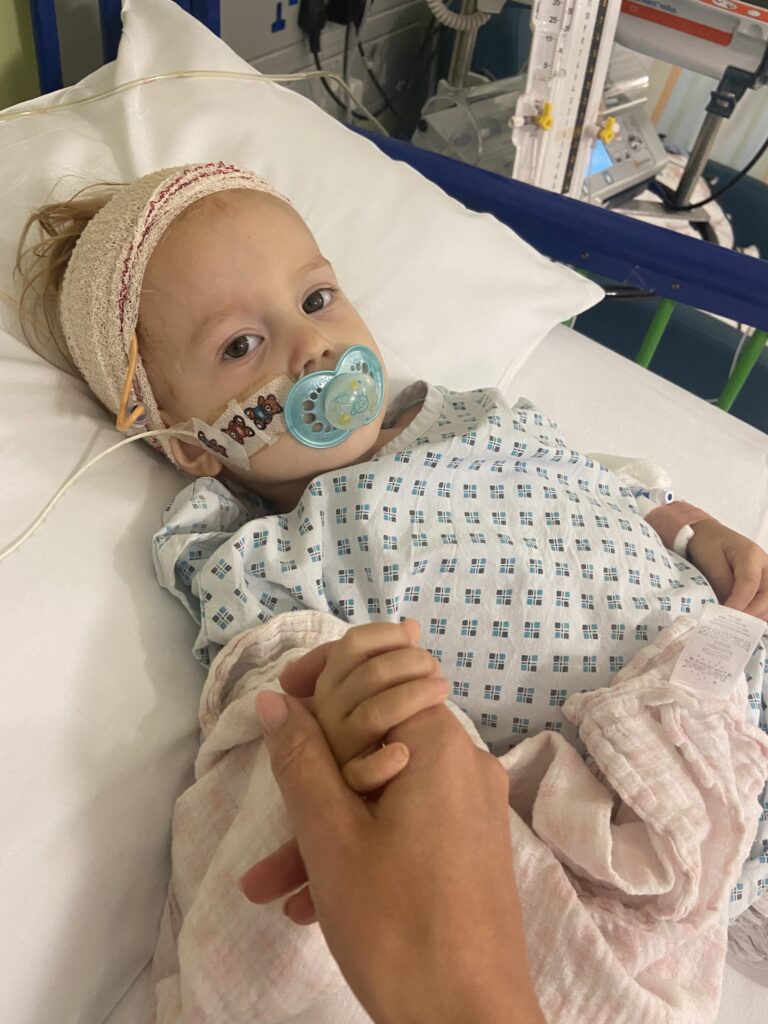
Temperature spiking
On 20 March Adam took her to the park opposite GOSH, and that evening she spiked a temperature. That wasn’t unusual, but the team could tell it was more serious than a normal spike. The temperature wasn’t responding to paracetamol or anti-biotics and the team suspected sepsis so monitored her all night and were in contact with paediatric intensive care. First thing the next morning I noticed her heart rate was dropping quickly, I told Adam and he said, ‘oh my God, she’s gone stiff’. The resus nurse pulled the emergency button and about 20 people rushed in, putting oxygen on her, laying her out on the bed. She’d had a peri-arrest, so her heart hadn’t stopped but she needed help breathing. Within minutes we were taken into intensive care and told they suspected she had a line infection and they needed to get it out of her immediately. This line infection was later confirmed as a very serious bacterial infection in her Hickman line that caused severe sepsis. Before they could take it out though, they needed to put more lines in her to administer the medication. The only place they could get the emergency cannulas was in her armpits because the rest of her limbs had already started to shut down. She had a purple rash all over her arms and legs and feet. Suddenly she went into cardiac arrest. Afterwards, we found out her heart stopped for up to a minute, but they were doing chest compressions for about four minutes. It was a really long four minutes and, in that moment, we really thought we’d lost her.
Ringing the end of treatment bell
They managed to bring her back, and got the line out, at which point we saw an immediate improvement and the medication started to work. Like always she bounced back so quickly. This all happened on the Tuesday, and by the Friday we were out of intensive care and back on the oncology ward. She amazed everybody. The following Tuesday a physiotherapist came in and they were really happy with her progress. We weren’t expecting her to get out of bed, but she wanted to get on the floor and play. A week later, on 12 April, we were discharged and on the 17 she had an MRI scan which incredibly came back clear, and she rang the end of treatment bell. Obviously, our hope was that all this gruelling treatment had cured her, and the plan was to monitor her with scans every three months. She still needed a lot of rehabilitation, and was immunocompromised until end of May, which was three months after her stem cells. So, we just did nice things at home as a family and at the end of May she had the PICC line taken out. That felt like a big step because it was always a big infection risk, so we were hopeful for her immune system getting stronger from that point.

Spending time together as a family
She had a speech therapist from the NHS come out to do an assessment. In some areas Orla was a little behind, but the wait for therapy was up to December. Luckily with private health insurance we were able to start this earlier. We also had one physio session, but the therapist said ‘she doesn’t need this, she’s doing amazingly well’, and discharged her, which was great to hear. As an end of treatment celebration break, we went to Centre Parks in June as a family, with my mum and dad and Adam’s dad as well. She had a fantastic time, she was able to swim and run around, we went bowling and played on the little beach. It was just such a relief, and so nice, for us all to be together, and distanced from hospitals and treatment. The only thing was, she still wasn’t eating orally, she was still being fed by her peg. So, every few hours she would need to be attached for her milk. The doctors also said high dose chemo really attacks your taste buds so flavours and textures change and can become less appetising. In hindsight, I think the tumour was already re-growing at this point and may have been quashing her appetite.
Losing her balance
Orla was all set to start pre-school in September, and enjoyed the start of July at playgroups, and watching her sisters do their sports day. Then on Tuesday 11 July, I noticed Orla was a bit off balance. I spoke to one of her local specialist nurses and they offered to have a look at her, but I said I was probably overly worried. Her three-month scan was coming up the following week we were all a bit anxious and on edge, so I thought I was looking for things that weren’t there. A couple of days later I still felt she wasn’t herself and was a bit all over the place. Adam hadn’t noticed, but I mentioned it to him and on closer inspection he agreed he could see it too. So, on the Friday we took her to the Princess Alexandria hospital to put our minds at rest.
It was much worse than they first thought
The doctor said it could be a middle ear infection, but as they’re hard to diagnose they contacted GOSH. GOSH said because her MRI was on the following Tuesday, we should just hang tight for a few days. But then on Sunday morning, Adam and I heard her let out this cough. We looked at each other and instantly knew what had happened and that something was going on again. Like at the very beginning of all of this; there was a little patch of yellow bile on her bedding. We took her straight back to the local hospital for a CT scan, which was sent to the neurosurgeon at GOSH. They asked her to come back in to GOSH because there were signs of hydrocephalus (fluid build-up). I went to GOSH in an ambulance with Orla and Adam went back to the girls. When we arrived, they drained some of the fluid from her brain via the Omaya reservoir, which was still in her brain from before. The next day they drained more fluid and decided they needed to operate to put in a permanent shunt, and in the meantime got her moved up the MRI emergency list. When the scan came back, they realised not only was there a recurrence, but it was much worse than they first thought.
There’s no more treatment
Her original tumour was on the right-hand side in a solid lump, but the recurrence had metastasised and was all the way up the left side of her brain – and it was diffuse. It had even penetrated the lining of the brain, in a condition called leptomeningeal. There was also another tumour spot near her pituitary gland, and two on her spine. The surgeon said to us ‘I’m so sorry, but there’s nothing we can do to operate on this’.
At that point we knew nothing could cure her, and it was more about how much time we had with her. We met again with her oncology team GOSH, as well as a palliative care team, and somebody from our local Haven House Hospice, to show us what support we would need. We discussed different options, including more intense chemotherapy, but we knew we didn’t want to do anything else that would harm Orla. We wanted her to still be her, and to feel well for as long as possible. We didn’t want her stuck in a hospital feeling awful, it’s no life. We had to stay at GOSH until Tuesday 25 July, just while her symptoms stabilised, and then decided to take her home. She wasn’t tolerating her medications orally so she had to go on a syringe driver with anti-sickness medication.
Everybody came together to celebrate Orla
On the Saturday, we decided to have a little get together for close family and friends. We weren’t sure if Orla would be up to it; she couldn’t walk anymore and could barely sit unaided. It was also a struggle for her to talk. But we carried her in, and Adam and I took turns just holding her. Everybody came together to celebrate her, we wanted everybody to be happy for her, and they were. It was just such a lovely day and we all made some beautiful memories. The following week, we decided we would all stay home until Orla’s time came and had medical staff coming in every day to help. But we made it as fun as we could for her; we had some Disney princesses in to see her, she had fun with her sisters, and we had a company take some castings of her feet and hands.
Positive experience at the Hospice
On Tuesday 8 August Orla started ‘posturing’, having little seizures and strange movements, so we went to Haven House Hospice. Orla then passed away on 12 August 2023. The hospice was a positive experience; we were all together and the pressure was off us. There were activities for the girls; music, yoga, woodland to play in and explore, and it was very peaceful and calm. We were able to take Orla outside in the sunshine and just be together. It was very hard, but we’re glad we made the decision to go there when we did. We will always love Orla and we’ll always talk about her and keep her memory alive. She was so strong and courageous; such an inspiration to everybody who knew her.

Sharing Orla’s Story
From the point we went to GOSH thinking something was wrong, to Orla passing, it was only about three and a half weeks. It was all so quick, and nobody expected it because she’d been doing so well. We know the type of medulloblastoma Orla had was really favourable to treatment, and it has about an 80% survival rate. We also know because of the rare mutation the cancer had, the doctors didn’t know exactly how best to treat Orla. Given how aggressively it came back, we really think that mutation was the driver in this relapse. We don’t want this to be the end, we want to keep telling her story and will create a legacy for her, to try to push for more research and help other families in the future going through this.
Naomi, Orla’s mum, December 2023
How you can help
If you’ve been touched by Orla’s journey, help us invest in the high quality research that really matters which would otherwise go unfunded.
Have you or a family member been affected by childhood cancer?
Many of our supporters have been affected by childhood cancer – either through family, friends or their own personal experience. These patient stories can help inspire others to get involved with us, or can support our media work. If you have a story that you would like to tell,
Other stories
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.