New cancer cell screening significantly improves treatment for children with leukaemia
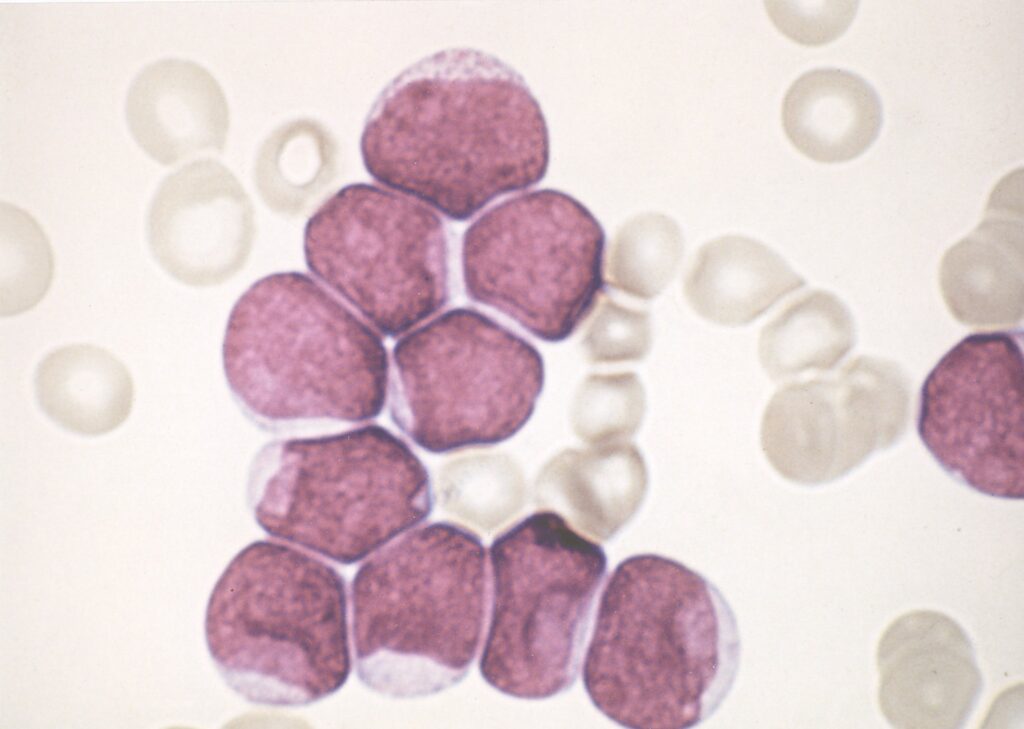
- New findings from groundbreaking childhood leukaemia trial (involving more than 2,500 children over eight years) shows combining MRD analysis with genetic profiling can significantly improve accuracy of predicting relapse in young patients, allowing clinicians to more accurately determine the correct level of chemotherapy required
- Minimal residual disease (MRD) is the name given to the measure of the amount of disease remaining in the patient during and after treatment when the patient is in remission (no symptoms or signs of disease). Such cells are the major cause of relapse in leukaemia
- Findings have already led to more tailored treatment options for children diagnosed with acute lymphoblastic leukaemia (ALL), the most common form of childhood cancer, with around 50 children a year currently benefitting from less toxic treatment
- The analysis also improves the ability to identify those with the highest risk of relapse – for whom five-year survival is just 60% – who may respond better to new types of treatment
- This approach has helped drive survival for children with acute lymphoblastic leukaemia above 90% – but the highly toxic treatment can have devastating short and long-term side effects for young patients
The research, by scientists at Newcastle University and doctors at Great Ormond Street Hospital and the Bristol Royal Hospital for Children, was funded by Bloodwise and Children with Cancer UK, and was published in the Journal of Clinical Oncology.Methods currently used to guide intensity of treatment for each child relies heavily on a test – known as minimal residual disease (MRD) – that measures levels of leukaemia cells remaining in the blood after the first month of chemotherapy.MRD gives a clear indication of how quickly a patient is responding to treatment. Children are placed into ‘low risk’ or ‘high risk’ treatment regimes, based on whether the number of leukaemia cells detected by their MRD test is above or below a single threshold.A team led by Professor Anthony Moorman, from the Northern Institute for Cancer Research, Newcastle University, analysed leukaemia cells from more than 2,500 children whose treatment had been guided by the MRD test between 2003 and 2011.The research has shown that, by combining the results of MRD analysis with genetic profiling doctors will be able to significantly improve the accuracy of predicting relapse of the disease and improving treatment options.The findings have already led to changes to treatment tailoring for newly diagnosed children, with around half of youngsters with good risk genetics being spared intensive treatment. The results may also be used to identify those children at the highest risk of relapse who would benefit most from new types of treatment, such as CAR-T cell therapy.Five-year survival for children diagnosed with the most common form of childhood cancer, acute lymphoblastic leukaemia (ALL), is now above 90%, while over 80% will survive in the long term. Treatment remains highly toxic, however, and can have severe short and long-term side effects, such as problems with fertility and heart problems in later life. The outlook is much poorer for those children whose disease relapses, with fewer than six in 10 children surviving longer than five years.Anthony Moorman, a Professor of Genetic Epidemiology, who co-leads the Leukaemia Research Cytogenetics Group at Newcastle University, said: “This study indicates that using a traditional MRD threshold to assign patients to different treatment groups should be refined with the integration of detailed genetic testing, to more accurately identify children with a lower or higher risk of relapse.
“Taking into account key genetic abnormalities that influence outcome will ensure that MRD thresholds for more or less intensive chemotherapy are more flexible and each child gets the most appropriate treatment.
“The idea of combining or integrating MRD and genetic information to refine the allocation of patients to different risk groups has been fully adopted in the next clinical trial, which is currently being designed and will hopefully begin in late 2018.
“Risk stratification is a key component of improving survival rates and reducing side-effects for children with leukaemia.”
Cliff O’Gorman, Chief Executive of Children with Cancer UK, said: “By developing a new way of interpreting MRD, we can significantly improve the accuracy of predicting how likely it is that a child with leukaemia will relapse. This has made more personalised treatment a possibility for young patients since we launched the trial in 2003, and helped to drive five-year survival for childhood acute lymphoblastic leukaemia above 90%.”
“But there is still much more to do. Children and young people diagnosed with cancer face aggressive treatments that can have a long-term impact on their health and well-being. It is crucial that we build on this breakthrough and continue to fund further studies and clinical trials to develop kinder, more effective treatment for young cancer patients in the UK.”
Dr Alasdair Rankin, Director of Research at Bloodwise, said: “Current treatments for children with leukaemia are highly toxic and can have devastating side effects both in the short and the long term. New ways to reduce treatment intensity, without reducing chances of survival, are desperately needed. This study represents another advance in personalising care and should mean that more children get the right treatment for them.”
Dr David O’Connor, Consultant Paediatrician in Haematology at Great Ormond Street Hospital, said: “Through this new research we have been able to take an important step forward to identify, earlier on, leukaemia patients who require more targeted therapy. This study suggests that early detection of patients’ specific treatment needs can improve patient outcomes, and reduce the risk of relapse and complications for those patients identified. This study represents an exciting advance in personalised medicine.”
About the research
The researchers divided children into groups depending on whether their leukaemia cells contained genetic abnormalities known to be associated with a ‘good’, ‘intermediate’ or ‘high risk’ of relapse. While children’s genetic risk of relapse broadly corresponded with their MRD test – assigned risk category, this was not always the case. The study found that children who had a ‘good risk’ genetic profile but whose blood was made up of between 0.01 and 0.1% leukaemia cells – just above the MRD threshold – actually had excellent chances of survival whether they were given standard treatment or intensive treatment. As a result of the findings, the MRD threshold at which children who are cytogenetic ‘good risk’ are treated with the most intensive treatment has now been raised, reducing treatment toxicity for around 50 children a year in the UK, without compromising their chances of survival. The study also identified a group of children currently treated with low intensity chemotherapy as a result of their low MRD test results who also have high risk genetics and who experience high rates of relapse. Indeed, nearly all children in the high risk genetics group who did not have a negative MRD result a month after treatment had very high relapse rates and may respond better to new types of treatment. By examining children’s MRD test results on a sliding scale, instead of whether they were simply above or below a certain threshold, the large-scale study demonstrated that children with very high levels of MRD treated with intensive treatment were much more likely to relapse than children who were just above the threshold. ENDS For further information please contact Hamir Patel or telephone 07771 780 946
Other stories
We have lots of information to help you learn more about childhood cancer. From specific cancer types, to treatments and causes.